Hashimoto’s Thyroiditis Diet: What to Eat + Anti-Inflammatory Guide
If you’ve been diagnosed with Hashimoto’s thyroiditis, or suspect a thyroid issue, you’re likely wondering one thing:
What should I eat to feel better?
Hashimoto’s thyroiditis is a chronic autoimmune condition in which the immune system mistakenly attacks the thyroid gland, leading to inflammation and reduced thyroid hormone production over time. It’s the most common cause of hypothyroidism (low thyroid function).
The condition is named after Dr. Hakaru Hashimoto, the physician who first described it in 1912. It’s also known as autoimmune thyroiditis or chronic lymphocytic thyroiditis.
Like many autoimmune conditions, Hashimoto’s doesn’t happen overnight. It develops from a combination of genetic susceptibility and environmental triggers, including nutrition, inflammation, and lifestyle factors.
If you’re newer to this way of eating, this breakdown of an anti-inflammatory eating pattern can help you understand how these pieces fit together in real life.
→ Dive deeper into a comprehensive guide on what an anti-inflammatory diet is (and isn’t)
→ If you want a simple, visual starting point, you can download my free anti-inflammatory food list to see exactly what foods to focus on.
While there’s no single perfect diet or cure, research continues to show that an anti-inflammatory eating pattern (like the Mediterranean diet) can support thyroid health, help regulate the immune system, and improve overall health.
In this article, you’ll learn:
- What Hashimoto’s thyroiditis is and how it affects the body
- How diet and inflammation are connected
- What foods to focus on (and what to limit)
- Simple, realistic ways to start eating in a way that supports your thyroid and prevents further damage
Because this doesn’t have to be complicated, and you don’t have to overhaul everything to start feeling better.
What is Hashimoto’s Thyroiditis?
Hashimoto’s thyroiditis is an autoimmune condition, but what does that actually mean for your thyroid and overall health?
How Hashimoto’s Affects the Thyroid
Hashimoto’s thyroiditis is an autoimmune condition in which the body’s immune system mistakenly attacks the thyroid gland.
Over time, this immune response leads to:
- Enlargement of the thyroid gland as it becomes overrun with lymphocytes (a type of white blood cell)
- Progress and irreversible damage to thyroid cells
- Reduced ability of the thyroid to produce hormones
As this damage progresses over time, the thyroid becomes less efficient, leading to reduced thyroid function.
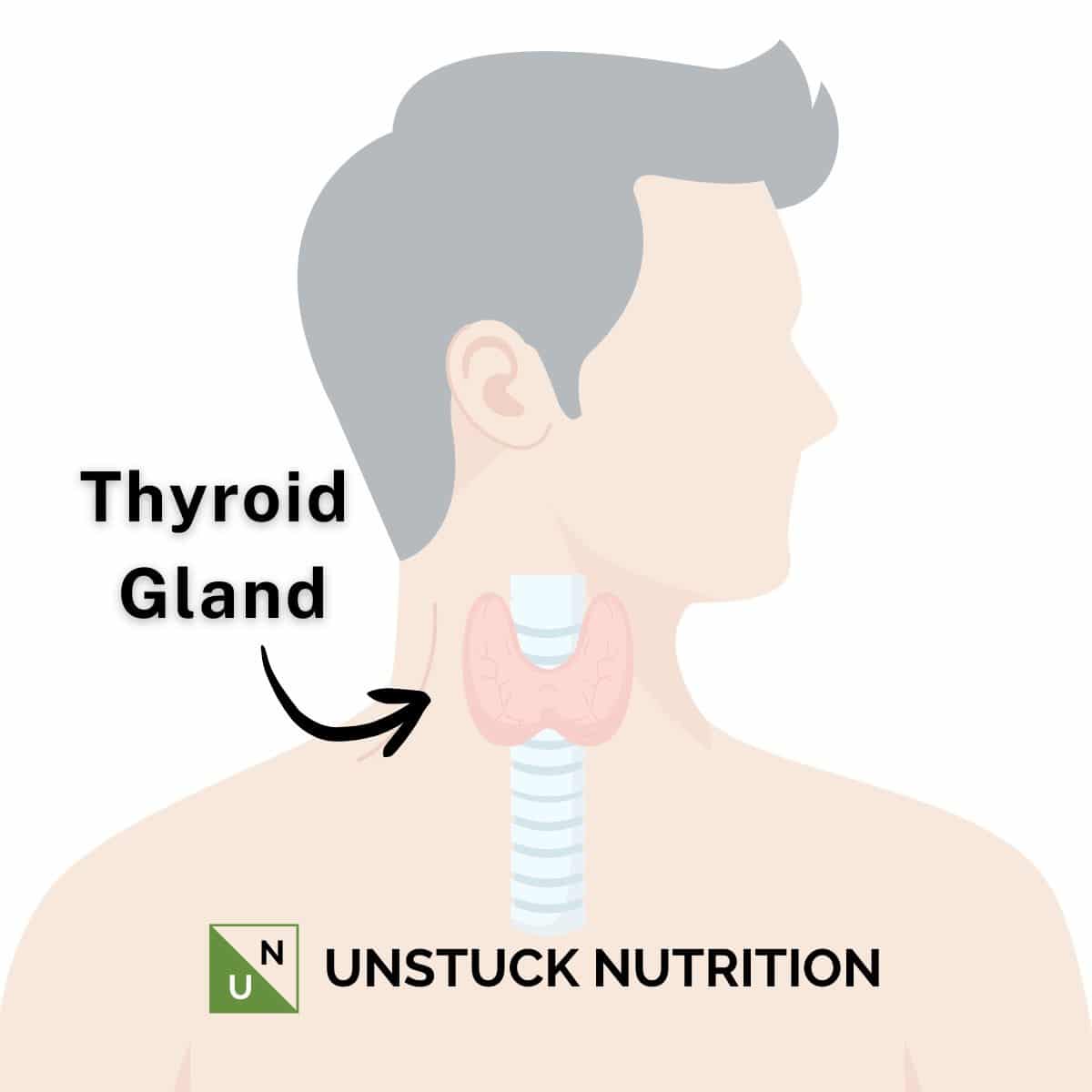
Why It Leads to Hypothyroidism
Because the thyroid gland produces hormones that regulate metabolism, energy, and many other functions, this ongoing damage eventually leads to hypothyroidism (low thyroid hormone levels).
Hashimoto’s is the most common cause of hypothyroidism.
When thyroid levels drop, it affects nearly every system in the body, including energy levels, metabolism, digestion, mood, and even blood sugar regulation.
What Causes Hashimoto’s Thyroiditis?
The development of Hashimoto’s thyroiditis is complicated. It reflects a complex interplay between genetic background and environmental triggers.
Genetic Risk Factors
This condition affects about 5% of American adults and is most common in women aged 45-55, although it can occur in anyone. A family history of thyroid disease increases the risk.
→ Learn more: Anti-Inflammatory Diet for Perimenopause
Environmental and Lifestyle Triggers
In people who are genetically susceptible, certain triggers may contribute to the development of autoimmune diseases. Hashimoto’s thyroiditis is associated with the following inflammatory triggers:
- Bacterial or viral infections
- Cigarette smoking
- Exposure to toxic chemicals (environmental toxins)
- Limited microbial exposure (sometimes referred to as living in an almost “sterile” environment
Nutritional Factors That May Play a Role
Diet can also influence inflammation and immune function.
Some factors that may play a role in Hashimoto’s for certain individuals include:
- Excessive iodine intake
- Inadequate selenium intake
- Gluten (particularly in those with celiac disease or sensitivity)
In addition, a typical Western-style diet (high in ultra-processed foods, unhealthy fats, added sugars, salt, and low in fiber) can further promote inflammation and may increase susceptibility to autoimmune conditions.
Common Symptoms of Hashimoto’s Hypothyroidism
As Hashimoto’s progresses and the thyroid becomes less able to produce hormones, symptoms of hypothyroidism begin to develop.
Because thyroid hormones affect nearly every system in the body, symptoms can vary widely, but often include:
- Cool, dry skin
- Coarse hair
- Loss of body hair
- Hoarse voice
- Edema (swelling)
- Bradycardia (slower than normal heart rate)
- Muscle cramps
- Gall stones
- Constipation
- Low or depressed mood
- Memory problems or difficulty concentrating
- Weight gain
- Joint stiffness
- Fatigue or tiredness
- Fertility problems
These symptoms typically develop gradually and may be subtle at first, which is why Hashimoto’s can go undiagnosed for years.
Why Symptoms Affect the Whole Body
Thyroid hormones play a key role in regulating metabolism and energy production, essentially, how your body uses carbohydrates, fats, and protein for fuel and repair.
They also influence:
- Brain function and mood
- Digestion
- Heart rate and circulation
- Fertility and hormone balance
Because of this, when thyroid hormone levels drop, the effects are not isolated to one area—they impact the entire body.
Related Conditions and Why They Matter
People with one autoimmune condition are more likely to develop another. Understanding these conditions can help with early screening and overall health management.
Hashimoto’s and Diabetes Risk
Hashimoto’s does not directly cause diabetes, but the two are closely connected.
- Type 1 diabetes (another autoimmune condition) often coexists with Hashimoto’s.
- Untreated hypothyroidism can slow metabolism and contribute to weight gain.
- It may also worsen insulin resistance, increasing the risk of type 2 diabetes.
Over time, these changes can affect your blood sugar management and overall metabolic health.
Hashimoto’s and Celiac Disease
People with Hashimoto’s thyroiditis have a higher rate of undiagnosed celiac disease, another autoimmune condition. Both conditions share common genetic factors.
Research suggests that between 2 and 8% of people with Hashimoto’s also have celiac disease, compared to about 1% of the general population. Celiac disease requires the complete elimination of gluten from the diet.
Screening for celiac disease may be helpful if symptoms are present, such as:
- Iron deficiency
- Digestive symptoms
- Family history of celiac disease.
Likewise, individuals with celiac disease may benefit from monitoring thyroid function.
Potential Complications of Untreated Hypothyroidism
When left untreated, hypothyroidism can lead to more serious health issues, including:
- Goiter (enlarged thyroid gland, located near the throat)
- Heart problems (high cholesterol, heart disease, irregular heartbeat, high blood pressure, enlarged heart)
- Fertility and pregnancy complications
- Myxedema (a rare but severe slowing of body functions)
Why Early Diagnosis and Management Matter
Early diagnosis and proper management of Hashimoto’s can help prevent complications and improve quality of life.
This often includes:
- Medical treatment (such as thyroid hormone replacement)
- Monitoring for related conditions
- Nutrition and lifestyle strategies to support overall health
Because while you can’t change the diagnosis, you can influence how you feel day to day.
How Diet Affects Hashimoto’s Thyroiditis
Hashimoto’s is of personal interest to me because my family members have this condition. I’ve spent a lot of time digging into the research, not as a cure, but as one tool to help support overall health and manage symptoms in a practical, sustainable way.
While diet doesn’t replace medical treatment, it can influence inflammation, immune function, and how you feel day to day.
The Link Between Inflammation and Autoimmune Disease
Research suggests that a typical Western diet and lifestyle may increase the risk of inflammatory and immune-related diseases.
This happens through several pathways, including:
- Low-grade chronic inflammation (learn more about how inflammation develops and impacts long-term health here)
- Immune system dysregulation
- Increased oxidative stress
- Imbalances in gut bacteria
These same underlying factors are linked to many chronic conditions, including type 2 diabetes, heart disease, and some cancers, as well as poor gut and brain health.
A Western-style eating pattern often includes:
- Excess calorie intake
- High trans fats (processed foods)
- Frequent ultra-processed foods (pre-packaged and fast food)
- High intake of fatty and processed meats
- Excess salt and added sugars (especially sugar-sweetened beverages)
- Low fiber intake (limited fruits, vegetables, beans, and whole grains)
Over time, this pattern can contribute to inflammation and may increase susceptibility to autoimmune conditions like Hashimoto’s.
The good news is that this also means diet is one area where you can make meaningful, supportive changes to counteract inflammation and autoimmunity. Research shows that nutrition approaches may improve thyroid markers.
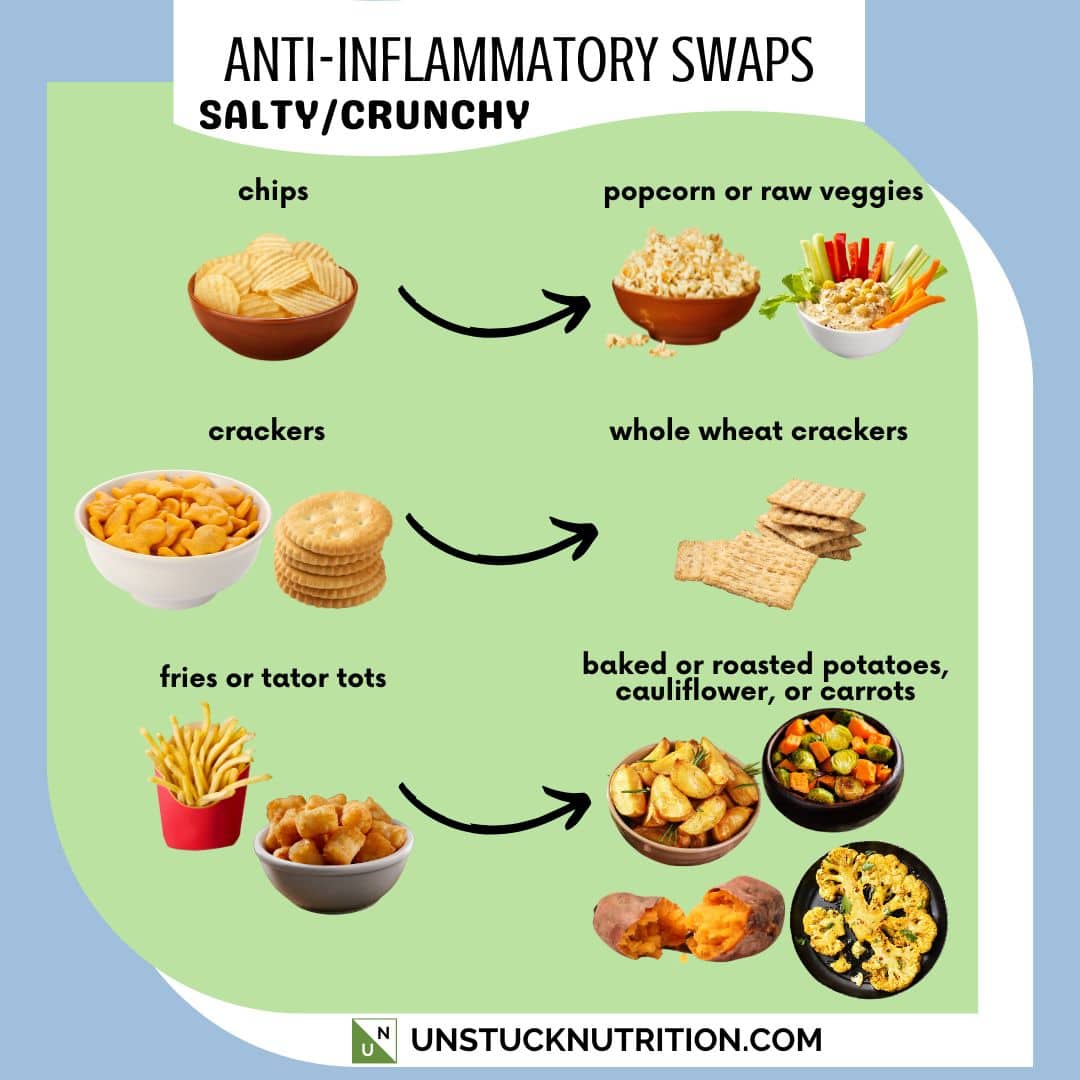
Why the Mediterranean Diet Is Often Recommended
Because of the link between inflammation and autoimmune disease, much of the research has focused on anti-inflammatory eating patterns.
One of the most well-studied approaches is the Mediterranean diet: a flexible, plant-based eating style that emphasizes whole, nutrient-dense foods.
This eating pattern is rich in:
- Antioxidants and polyphenols
- Fiber
- Healthy fats
- Vitamins and minerals
Key components of a Mediterranean-style (anti-inflammatory) diet include:
- A high intake of vegetables, fruits, legumes, nuts, and whole grains
- Olive oil as the primary fat source
- Regular intake of fish and seafood
- Low to moderate amounts of dairy, poultry, and eggs
- Limited red and processed meats
- Minimal added sugars and highly processed foods
This eating pattern has been shown to:
- Support gut health and microbiome balance
- Reduce inflammation
- Improve markers related to heart disease, diabetes, and metabolic health
Research on Hashimoto’s is still emerging, but given its strong anti-inflammatory effects and overall health benefits, it’s a practical, low-risk approach to support thyroid health and well-being.
What About Gluten?
A gluten-free diet is often discussed in relation to Hashimoto’s due to the increased prevalence of celiac disease in this population.
However, routine gluten elimination isn’t recommended for everyone.
- It can be beneficial for individuals with celiac disease or confirmed gluten sensitivity
- Helpful for those where gluten worsens GI symptoms, joint pain, rashes, or fatigue
- But for others, removing gluten unnecessarily may add restriction without clear benefit
- It may also increase the risk of nutrient gaps if not well-planned
Some research indicates that individuals with Hashimoto’s are more likely to have food intolerances, including gluten-containing foods, and may see improvements in their thyroid antibodies after removing gluten. Gluten may add fuel to an already overactive immune system for people with Hashimoto’s.
The part of gluten that causes the trouble is gliadin, which is very resistant to digestion, leaving large fragments in the gut. The gliadin fragments can trigger strong immune responses that activate inflammatory signals in the gut and damage the intestinal lining.
For most people, the most effective approach is to start with a consistent anti-inflammatory eating pattern first (see exactly how to build that here), then personalize from there.
Once inflammation, energy, and blood sugar are more stable, you can begin to evaluate potential trigger foods like gluten, dairy, or eggs more strategically.
This “stabilize first, then personalize” approach helps you avoid unnecessary restriction while still identifying what truly impacts your symptoms.
What Does the Research Say About Diet and Hashimoto’s?
The growing interest in nutrition and autoimmune disease has led to an increasing number of studies exploring how dietary patterns may influence Hashimoto’s thyroiditis.
While there’s no single “perfect” diet, research suggests that more anti-inflammatory eating patterns are associated with better thyroid and inflammatory markers.
Below is a summary of current research on different nutrition approaches and their potential impact on Hashimoto’s.
If you’re not interested in the research details, feel free to skip ahead. I’ll share the key takeaways after the table!
Most of the research in this area is still emerging, including small clinical trials and observational studies. While not definitive, the findings provide helpful direction for practical dietary strategies.
| Nutrition Topic | Study Title | Study Type & Size | Key Findings |
| Anti-inflammatory diet pattern | Dietary Inflammatory Index, Antioxidant Capacity & Hashimoto’s | Case-control observational study, 230 adults | Diets with higher anti-inflammatory properties were associated with lower rates of Hashimoto’s thyroiditis. |
| Diet quality & thyroid function | Dietary Inflammatory Index and Thyroid Function in Hashimoto’s | Observational study, 149 adults | Higher intake of pro-inflammatory diets was linked with worse thyroid function and inflammation markers. |
| Mediterranean diet | Mediterranean Diet in Hashimoto’s Thyroiditis | Randomized controlled trial, 40 female adults | Mediterranean diet improved thyroid markers, inflammation, BMI, cholesterol, and quality of life. Greater improvements were seen in those with hypothyroidism on medication. |
| Mediterranean + goitrogen (thyroid markers) reduction | Same RCT as above | Randomized controlled trial, 40 adults | Both groups improved, suggesting that overall diet quality is more important than focusing on individual “avoid” foods. |
| Low-carbohydrate diet | Low-Carb Therapy in Hashimoto’s Thyroiditis | Controlled trial, 40 adults (6 months) | A low-carb diet (12-15% carb, 50-60% protein, 25-30% fat) reduced thyroid autoantibodies and markers of inflammation, suggesting reduced thyroid tissue inflammation. |
| Mediterranean vs. gluten-free diet | Diet Comparison in Autoimmune Thyroid Disease | Randomized controlled trial, 40 adults (4 groups, 12 weeks) | The Mediterranean diet showed the most consistent improvements in thyroid markers. A gluten-free diet showed greater changes in body composition but had a lesser impact on thyroid markers. |
| Gluten and Hashimoto’s | The Role of Gluten in the Development of Autoimmune Thyroid Diseases | Narrative review of human( at least 10 studies with about 300 adults), animal, and mechanistic studies published between 2000 and 2024 | Gluten may worsen autoimmune thyroid disease in susceptible individuals through gut dysbiosis, increased intestinal permeability, and immune cross‑reactivity A gluten‑free diet appears clearly beneficial in patients with celiac disease and potentially helpful in select non‑celiac patients, but is not universally required for all individuals with Hashimoto’s thyroiditis |
| Oxidative stress & diet patterns | Mediterranean vs. Gluten-Free Diet on Oxidative Stress | Randomized controlled trial, 45 adults | The Mediterranean diet improved antioxidant markers. Gluten-free and control diets showed no improvement in oxidative stress or thyroid markers. |
| Selenium supplementation | Selenium and Hashimoto’s Thyroiditis (Meta-analysis) | Systematic review of 35 studies (>3,000 adults) | Selenium may reduce immune activity and improve thyroid markers, particularly in individuals not on thyroid medication. Most studies used 200mcg/day of selenium yeast or sodium selenite for 3-6 months. The upper limit for selenium is 400 mcg/day for adults. |
| Vitamin D status | Vitamin D and Hashimoto’s Thyroiditis Review | Review article | Vitamin D deficiency is common in Hashimoto’s. Correcting the deficiency may reduce immune activity, especially in early or milder disease. Harder to determine if supplementation helps once Hashimoto’s is more advanced or if medication (thyroid replacement) is already in use. |
Research Highlights
The short answer is yes, anti-inflammatory diets can help with Hashimoto’s. While the research is still emerging, a few consistent themes stand out:
- Diets with lower inflammatory potential are associated with better thyroid and immune markers
- The Mediterranean diet shows the most consistent benefits for overall health and inflammation
- A gluten-free diet may help some individuals, particularly those with celiac disease or sensitivity, but it isn’t necessary for everyone
- Nutrients like selenium and vitamin D may play a supportive role, especially if deficiencies are present
Overall, the goal isn’t perfection or restriction; it’s building a consistent, anti-inflammatory eating pattern that supports your body over time and benefits overall health and well-being.
Why This Matters Beyond Hashimoto’s
Chronic disease is common in the United States and often overlaps with inflammatory and metabolic conditions.
For context, the CDC estimates that about 129 million Americans have at least one major chronic disease, and among older adults, that number rises to over 85%.
Many of these conditions, including heart disease, type 2 diabetes, insulin resistance, obesity, metabolic syndrome, cognitive decline, and certain cancers, share underlying links with chronic inflammation and metabolic dysfunction.
This is one reason dietary patterns like the anti-inflammatory or Mediterranean-style diet are so widely studied; they support multiple systems in the body, not just one condition.
Bringing It Back to Hashimoto’s
While diet is not a cure for Hashimoto’s thyroiditis, it can be one supportive tool alongside medical treatment and lifestyle habits.
Small, consistent changes in how you eat can help reduce inflammation, stabilize energy, and support overall metabolic health over time.
Next, we’ll look at practical ways to apply this in everyday life.
What to Eat for Hashimoto’s (Simple Anti-Inflammatory Guide)
As you focus on the big picture of eating to support your thyroid health, an anti-inflammatory diet is the first and most impactful step. Focus on addition before subtraction.
Hashimoto’s is influenced more by overall inflammatory and metabolic dietary patterns than by single problem foods.
The evidence supports an anti‑inflammatory, antioxidant‑rich eating pattern with individualized adjustments (specific food removals), rather than broad restriction.
Some individuals with Hashimoto’s find certain foods are triggers for them, such as gluten or eggs, and these will be discussed in greater detail below.
Each person is unique, and some find removing certain foods makes a difference, whereas others find minimal improvement and that it’s restrictive. Experimentation and time will help reveal which foods make you feel your best and which ones trigger symptoms.
Anti-Inflammatory Foods That Support Thyroid Health
Nutrition research continues to highlight the powerful benefits of plant-based foods — fruits, vegetables, high-fiber carbohydrates, healthy fats, herbs, spices, and even beverages like coffee and tea. A 2025 study found that people following an anti-inflammatory diet experience marked improvements in thyroid function, suggesting a more regulated immune response. Key food categories to focus on:
1. Plant foods (fruits and vegetables)
Focus on berries, grapes, citrus fruits like oranges, cherries, bell peppers, carrots, cooked broccoli, leafy greens like spinach, chard, kale, and arugula.
2. Fiber-rich carbohydrates (whole grains and legumes)
Focus on brown rice, quinoa, buckwheat, lentils, chickpeas, beans, and bean-based pasta. If no gluten issues, oats, whole grain pasta, bread, or cereal.
3. Healthy fats (omega-3 and unsaturated fats)
Focus on nuts, seeds (flax or chia), avocados, olives, olive oil, and fatty fish.
4. Protein foods that support metabolism
Focus on salmon, sardines, chicken breast, turkey, fish, and fermented dairy like yogurt or kefir (if tolerated).
5. Herbs, spices, tea, and coffee
Focus on garlic, turmeric, ginger, cinnamon, and unsweetened green tea and coffee.

An anti-inflammatory diet is built primarily on these foods, not because of a single nutrient, but because of how they work together to reduce inflammation throughout the body.
Rather than focusing on a single “superfood,” the goal is to regularly include a variety of high-impact foods. Once you have established a sustainable anti-inflammatory eating pattern, take time to investigate potential food triggers.
→ For a complete breakdown of which foods to focus on and why they work, see The Best Anti-Inflammatory Foods to Eat After 40
→ Want a done-for-you reference? Grab the Printable Anti-Inflammatory Food List
So what about foods to avoid with Hashimoto’s? The answer has two parts: a few Hashimoto’s-specific considerations worth knowing, and the general inflammation drivers that apply to most chronic conditions. Here’s a practical look at both.
Foods to Limit (Without Over-Restricting)
Some research has shown that individuals with Hashimoto’s are more likely to develop more food intolerances (IgG food antibodies) than the general population. However, IgG reflects immune overexposure or reactivity, not allergies. It likely reflects immune dysregulation and poor gut-immune interactions rather than a true allergy.
Monitor more common trigger foods, such as gluten, dairy, soy, eggs, and cruciferous vegetables, for worsening symptoms. Then, experiment with an elimination diet: remove potential triggers for 4 to 6 weeks, then reintroduce a food one at a time and monitor for any symptom return. If symptoms return, remove that specific food.
In the past, cruciferous vegetables were routinely restricted for people with thyroid issues due to concerns about compounds that may interfere with iodine uptake.
However, current research shows these vegetables offer significant anti-inflammatory and antioxidant benefits, even for individuals with thyroid conditions.
If you have concerns, lightly cooking them (steaming or sautéing for 2–4 minutes) reduces these compounds (goitrin) while preserving 85-95% of the beneficial nutrients.
→ Learn more about raw vs. cooked greens here: Raw vs. Cooked Greens: Simple Strategies for Real-Life Eating
General inflammation drivers for chronic conditions that should be avoided:
- High intake of ultra-processed foods is linked with worse thyroid function and inflammation
- Refined carbohydrates eaten alone (without protein or fat) and frequently
- Excess added sugar from drinks, desserts, and packaged foods
- Processed meats and excess red meat
- Diets high in certain omega-6 fats from highly processed oils
- Alcohol consumption may trigger inflammation and is often high in added sugar
→ For a clear, organized reference, download my printable anti-inflammatory food list (what to eat more of and what to limit)
How to Build an Anti-Inflammatory Plate for Thyroid Health
Building an anti-inflammatory plate doesn’t require calorie counting or complicated meal planning. It comes down to a simple formula that naturally supports blood sugar balance, reduces inflammation, and keeps energy steady throughout the day.
- Fill half your plate with non-starchy vegetables. Think leafy greens, bell peppers, broccoli, carrots, zucchini, or whatever is in season. Sauté or lightly steam if you are concerned about goitrins. These provide the fiber, antioxidants, and polyphenols that drive the anti-inflammatory benefits of this eating pattern.
- Fill one quarter with a quality protein. Salmon, sardines, chicken, turkey, eggs (if tolerated), or legumes like lentils and chickpeas. Protein supports metabolism, stabilizes blood sugar, and helps with the fatigue that often accompanies Hashimoto’s.
- Fill the remaining quarter with a fiber-rich carbohydrate. Brown rice, quinoa, sweet potato, fruits, and if no gluten issues, include oats or whole-grain bread. Pairing carbohydrates with protein and fat slows glucose absorption and prevents the blood sugar spikes that drive inflammation.
- Add a healthy fat. A drizzle of olive oil, a few slices of avocado, or a small handful of nuts or seeds. Healthy fats support the absorption of fat-soluble nutrients.

This plate works at any meal and is flexible enough to accommodate individual food sensitivities or preferences.
→ For a step-by-step walkthrough of how to apply this formula, see my Anti-Inflammatory Plate Method.
Easy Meal Ideas for Busy Days
Following an anti-inflammatory eating pattern doesn’t have to mean elaborate cooking. Here are simple combinations that follow the plate method and work for real, busy days:
Breakfast: Your first opportunity of the day to influence both inflammation and blood sugar. Simple options that follow the plate formula include oatmeal topped with walnuts and berries OR scrambled eggs with spinach and avocado on whole-grain toast OR Greek yogurt with ground flaxseed and fruit.
→ For a full breakdown of the anti-inflammatory breakfast formula, grab-and-go ideas, and a sample breakfast week, see Best Anti-Inflammatory Breakfast for Women Over 40
Lunch: Mediterranean chickpea salad with chicken OR leftover salmon over brown rice with roasted vegetables.
Dinner: Baked salmon with roasted broccoli and quinoa OR chicken stir-fry with mixed vegetables over brown rice OR turkey and vegetable-stuffed sweet potato.
→ For more dinner ideas using the plate method, see Anti-Inflammatory Dinners: How to Quickly Plan a Meal
Snacks: Snacking is one of the easiest places to make an anti-inflammatory swap, and it adds up. Keep simple combinations on hand, like No-Mess, No-Bake Energy Bites OR hummus with sliced bell peppers and carrots OR a small handful of mixed nuts with fruit.
→ For 10 ready-to-buy options that require no prep, see 10 Best Anti-Inflammatory Snacks to Buy, According to a Dietitian
Blood Sugar, Inflammation, and Thyroid Health
One often-overlooked piece of managing Hashimoto’s is blood sugar balance.
Thyroid hormones play a key role in metabolism, including how your body processes carbohydrates and regulates glucose. When thyroid function slows, it can contribute to insulin resistance, unstable blood sugar (this is where many people get stuck—here’s how to balance blood sugar naturally), and increased inflammation.
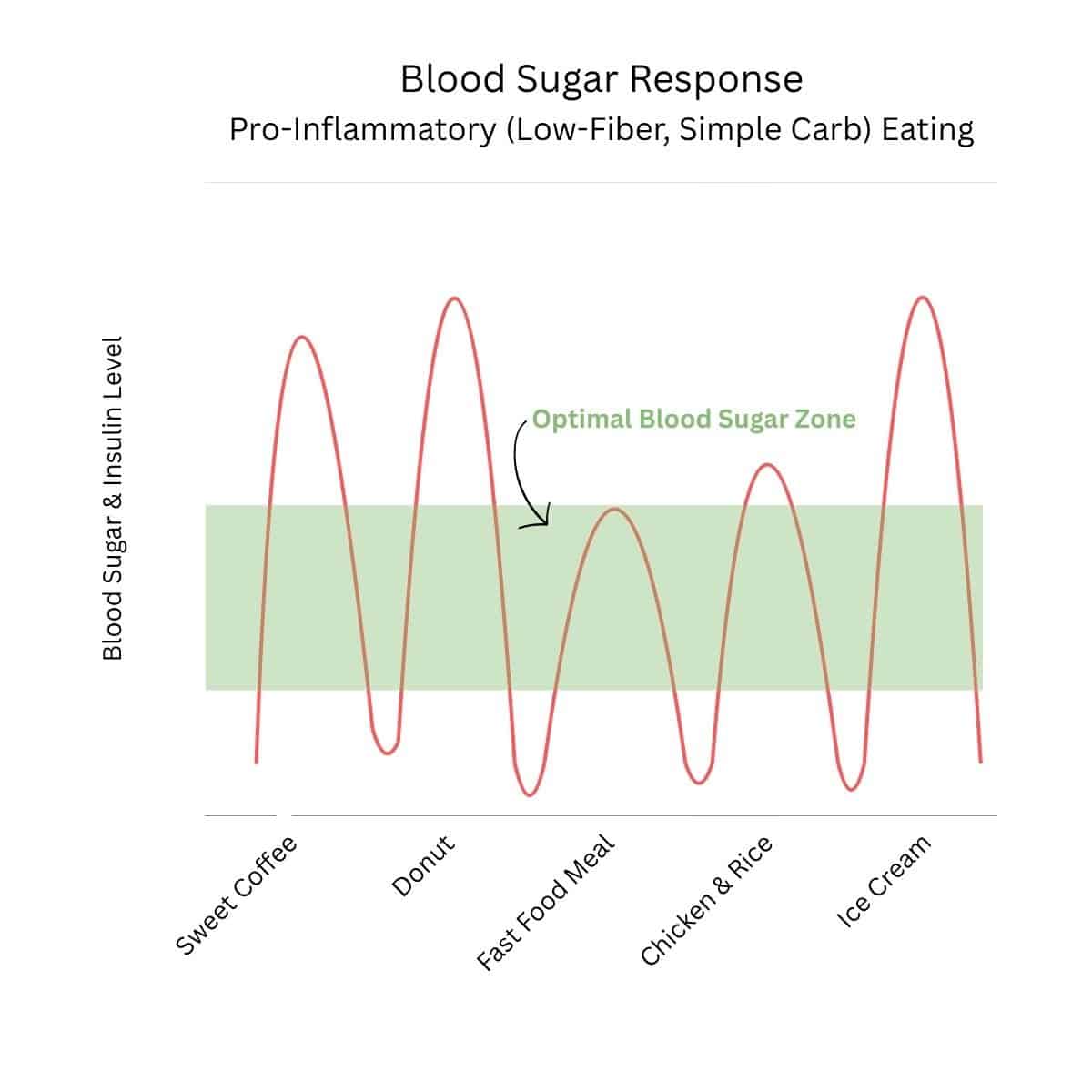
At the same time, blood sugar swings (frequent spikes and crashes) can:
- Increase inflammatory signaling
- Disrupt energy levels
- Worsen fatigue and cravings
- Add stress to an already dysregulated immune system
This creates a feedback loop where blood sugar instability and inflammation reinforce each other, making symptoms harder to manage.
Why Blood Sugar Balance Matters for Hashimoto’s
Research shows that people with hypothyroidism and Hashimoto’s are more likely to experience insulin resistance and impaired glucose metabolism.
Over time, this can increase the risk of:
- Type 2 diabetes
- Weight gain
- Metabolic syndrome
- Cardiovascular disease
The key takeaway:
The same habits that support blood sugar balance also support thyroid health and reduce inflammation.

→ Blood sugar swings don’t just affect energy—they also increase stress hormones like cortisol, which can further drive inflammation (I explain this connection in detail in my stress, cortisol, and inflammation article for midlife women).
Simple Ways to Stabilize Blood Sugar Daily
You don’t need a complicated plan. Focus on a few consistent habits:
- Pair carbohydrates with protein and healthy fats
- Avoid eating refined carbs on their own
- Include fiber-rich foods at every meal
- Don’t skip meals (especially breakfast)
- Build balanced plates (this is the same approach I use in my anti-inflammatory plate method)
These small shifts help maintain steady energy levels, reduce inflammation, and support overall metabolic health. This becomes even more important in midlife, where hormonal shifts can amplify both inflammation and blood sugar instability (read more in my anti-inflammatory diet for perimenopause guide).
What Does the Research Say About Diet and Hashimoto’s?
Managing Hashimoto’s thyroiditis typically involves a combination of medical treatment and lifestyle strategies.
While medication, such as thyroid hormone replacement, is often necessary for life, nutrition can play a meaningful supportive role to help you feel better, reduce inflammation, improve thyroid function, reduce future damage, prevent other medical conditions.
An anti-inflammatory eating pattern has been associated with improvements in thyroid markers, immune activity, and overall health. However, it’s important to keep expectations realistic. Diet is not a substitute for medical treatment, but rather one tool that can support long-term health and symptom management.
Key Takeaways From Current Studies
While research is still emerging, several consistent themes stand out:
- Diets with lower inflammatory potential are associated with better thyroid and immune markers
- The Mediterranean diet shows the most consistent benefits for overall health and inflammation
- A gluten-free diet may help some individuals, particularly those with celiac disease or sensitivity, but it isn’t necessary for everyone
- Nutrients like selenium and vitamin D may play a supportive role, especially when deficiencies are present
Overall, the goal isn’t perfection or restriction. It’s building a consistent, anti-inflammatory eating pattern that supports your body over time and contributes to overall health and well-being.
Key Nutrients for Thyroid Support
When it comes to Hashimoto’s, two nutrients consistently show up in the research: selenium and vitamin D. Neither is a cure, but both may play a meaningful supporting role, especially if your levels are low.
Selenium and Thyroid Function
Selenium is an essential trace mineral that your thyroid gland depends on to function properly. Many of the enzymes involved in thyroid hormone production and protection against oxidative damage are selenoproteins.
A 2024 systematic review and meta-analysis of 35 randomized controlled trials found that selenium supplementation reduced thyroid peroxidase antibodies (TPOAb – the antibodies that drive the immune attack on the thyroid) in people with Hashimoto’s, regardless of whether they were on thyroid medication. In those not yet on medication, selenium also helped lower TSH levels. Doses above 100 mcg per day appeared most effective, with 200 mcg a common dosage, and the supplementation was well tolerated.
One important sidenote: if your selenium levels are already adequate, supplementing may not provide additional benefit and could carry risks at very high doses. Ask your provider to check your levels before adding a supplement.
If you’d rather focus on food first, several selenium-rich foods are already staples of an anti-inflammatory diet: Brazil nuts, salmon, tuna, cod, chicken, eggs, and sunflower seeds.
Vitamin D and Immune Health
Vitamin D does more than support bone health. It plays an active role in regulating your immune system, and that matters for Hashimoto’s.
A 2023 review outlines several ways vitamin D may help calm the autoimmune process in Hashimoto’s by assisting on multiple levels of the immune response to bring control.
The connection between low vitamin D and Hashimoto’s is well-documented. People with low vitamin D levels tend to have higher antibody levels, which can drive thyroid damage.
In terms of resolving deficiencies, vitamin D supplementation is encouraging. Most studies report significant improvement in immunological markers after supplementation. A large study found that participants who achieved optimal vitamin D levels saw meaningful reductions in antithyroid antibodies, and those with subclinical hypothyroidism saw a 72% reduction in that diagnosis at follow-up
Work with your provider to test, monitor, and correct an actual deficiency. If you’d prefer to focus on food first, vitamin D-rich foods that align with an anti-inflammatory eating pattern include salmon, sardines, trout, egg yolks, and certain mushrooms, particularly those exposed to UV light.
Practical Ways to Support Thyroid Health
While you can’t reverse the damage Hashimoto’s has already caused, you can take steps to support your thyroid, reduce inflammation, and protect your overall health going forward. Here’s what the research supports.
Medical Treatment and Monitoring
The thyroid gland and its ability to make thyroid hormones are irreversibly damaged in Hashimoto’s. Most people will likely require lifelong levothyroxine medication to ensure their bodies receive adequate thyroid hormone, which can help reduce side effects on metabolism, energy, mood, and other body systems. Work closely with your healthcare provider to manage your dosage and monitor thyroid hormone levels regularly.
Consider asking your provider about screening for celiac disease or gluten sensitivities since these two autoimmune diseases are genetically associated. For those who have both, a gluten-free diet can provide additional benefit beyond general anti-inflammatory eating.
Nutrition and Daily Habits That Help
An anti-inflammatory diet is one of the most practical tools you have. It won’t replace your medication, but consistent anti-inflammatory eating can help reduce inflammation, support immune function, stabilize energy levels, and lower your risk of related conditions like heart disease and type 2 diabetes.
Exercise and Thyroid Function
Regular physical activity is an underrated tool for thyroid health. A randomized controlled trial of 60 women with hypothyroidism found that aerobic, resistance, and combined exercise programs all improved thyroid function and quality of life. Resistance training produced the most significant improvements in thyroid function specifically, while the combination of aerobic and resistance exercise led to the greatest gains in overall quality of life.
The practical takeaway: aim for a mix of both. Even two to three days of strength training combined with regular walking or cardio can make a meaningful difference.
Blood Sugar and Insulin Resistance
Blood sugar and insulin resistance often get overlooked in Hashimoto’s care. People with Hashimoto’s and hypothyroidism may experience altered glucose metabolism, which can contribute to insulin resistance, chronic inflammation, and eventually metabolic syndrome or type 2 diabetes. Research has shown that individuals with hypothyroidism and Hashimoto’s have higher rates of insulin resistance and impaired glucose intolerance than healthy controls.
Annual blood sugar screening (such as the A1C test, which reflects your average blood sugar levels over the past 3 to 4 months) can help detect early signs of prediabetes. This is especially important because insulin resistance and inflammation are a two-way street: each can worsen the other.
The good news is that the anti-inflammatory eating pattern covered in this article is one of the most effective dietary strategies for supporting blood sugar balance, too. So the same habits that support your thyroid also support your metabolic health.
FAQs About Hashimoto’s Thyroiditis and Diet
Can diet cure Hashimoto’s?
No, a diet cannot cure Hashimoto’s thyroiditis. Damage to the thyroid gland is irreversible, and most people require lifelong thyroid hormone replacement medication.
However, an anti-inflammatory diet can be a supportive tool. It may help reduce inflammation, lower thyroid antibodies, support immune function, and lower the risk of related conditions like heart disease and type 2 diabetes. It is one tool in your toolbox for managing your overall health.
Should I go gluten-free with Hashimoto’s?
Not necessarily. A gluten-free diet is beneficial for people who also have celiac disease or confirmed gluten sensitivity. For others, the evidence is less clear. Some people with Hashimoto’s do notice improvements in symptoms or antibody levels after removing gluten.
Start by building a strong anti-inflammatory eating foundation. If symptoms persist, work with your provider to screen for celiac disease and then try eliminating gluten.
What is the best diet for Hashimoto’s?
The Mediterranean diet has the most consistent evidence for Hashimoto’s and almost all chronic conditions. This anti-inflammatory eating pattern is flexible and sustainable in the long term. Rather than following a rigid plan, focus on building an overall anti-inflammatory eating pattern that you can maintain consistently.
How long does it take to see results from diet changes?
Most people need at least four to six weeks of consistent anti-inflammatory eating before noticing meaningful changes in energy, digestion, or inflammation. Thyroid antibody levels, which reflect immune activity, tend to shift more slowly (often over three to six months).
Small daily habits compound over time, and the benefits extend well beyond thyroid health to your heart, metabolic health, and overall energy. Track how you feel week to week rather than looking for dramatic overnight changes.
→ For a detailed breakdown of what to track and what to expect at each stage, see How Long Does the Anti-Inflammatory Diet Take to Work?
Takeaways: How to Support Thyroid Health With Diet and Lifestyle
Hashimoto’s thyroiditis develops from a mix of genetic susceptibility and environmental triggers, leading to progressive thyroid damage and reduced thyroid hormone production.
You can’t change your diagnosis, but you can change your daily habits, starting with your next meal.
Focus first on building a consistent anti-inflammatory foundation. From there, you can personalize your approach based on how your body responds.
By combining anti-inflammatory nutrition, steady blood sugar, and targeted adjustments when needed, you can get UNstuck and better support your thyroid health long-term.