Quality sleep becomes more elusive for many women as they enter their late 30s, 40s, and 50s, and there’s a biological reason for that.
Sleep problems are incredibly common during the menopause transition. One study of over 3,000 women found that more than half of perimenopausal women experience chronic insomnia, compared to about one in three women before perimenopause begins. For women dealing with severe hot flashes, that number climbs above 80%.
Maybe you feel like nothing has changed on your end:
- You’re eating well
- Managing stress
- Stopping caffeine before noon
But your sleep feels less consistent and less restorative than it used to. You’re wide awake at 2 or 3 am, or waking drenched in sweat, unable to fall back asleep.
Hormonal shifts are one of the primary drivers. As estrogen fluctuates unpredictably and progesterone declines during perimenopause, your brain loses two of its most important sleep-regulating signals.
Research shows that drops in estrogen often predict higher cortisol levels the following morning, disrupting sleep quality, mood, and stress resilience before your day even begins. Declining progesterone removes one of the brain’s natural calming signals, making it easier to wake during the night and harder to fall back asleep.
If this sounds familiar, you may have already read about how these same hormonal shifts drive the stress-cortisol cycle in midlife. Poor sleep is part of that same system, just a different expression of the same underlying disruption. → Stress, Cortisol & Inflammation in Midlife Women
So let’s jump into what’s actually happening in your body, why it matters beyond just being tired, and some practical and effective ways to improve your sleep.
Why Sleep Changes in Midlife
How Hormonal Shifts Disrupt Sleep
It’s not just that you’re sleeping fewer hours; the quality of your sleep can decline, too, which impacts far more than energy levels. Poor sleep affects memory, mood, daytime functioning, immune health, and even systemic inflammation.
Both estrogen and progesterone help support deep, restorative sleep. As these hormones fluctuate and decline during perimenopause, sleep often becomes lighter, more fragmented, and less refreshing.
Estrogen fluctuations are often at their most erratic during perimenopause, sometimes showing up as subtle sleep disruptions years before periods fully stop. These unpredictable hormonal shifts can interfere with neural pathways that regulate sleep, mood, and cognitive function, and disrupt your body’s internal temperature regulation.
At the same time, fluctuating estrogen can trigger hot flashes and night sweats by disrupting the body’s temperature regulation system, leading to fragmented sleep and increased cortisol reactivity. Women with moderate to severe hot flashes are almost three times more likely to experience frequent nighttime awakenings than women without them.
Hot flashes are one of the most disruptive symptoms during the menopause transition and often worsen sleep fragmentation and inflammation. → Anti-Inflammatory Diet for Perimenopause: A Dietitian’s Complete Guide
And once you’re awake, falling back asleep may become more difficult, partly because of declining progesterone. Progesterone has a natural calming effect on the brain and nervous system. A 2021 systematic review found that oral micronized progesterone improved sleep outcomes in menopausal women, particularly by reducing nighttime wakefulness rather than increasing total sleep duration.
A 2019 review shares that neurological symptoms like sleep disruption and brain fog are the most common complaints of the menopausal transition, with negative effects on quality of life, productivity, and physical health.
Combined, these hormonal shifts and fragmented sleep can throw cortisol rhythms out of balance, a pattern I covered in depth → Stress, Cortisol & Inflammation in Midlife Women.
Instead of fully winding down at night, the nervous system can remain in a low-grade state of alertness, making it harder to maintain deep, restorative sleep.
Why This Isn’t Just “Normal Aging”
Poor sleep in midlife is common, but that doesn’t mean it’s inevitable or that you should just push through it.
Chronic sleep disruption compounds nearly every other perimenopause symptom you may already be managing. It worsens brain fog and concentration, increases cortisol and inflammatory markers, drives cravings for high-sugar foods, and makes weight management (and weight distribution) significantly harder. Over time, consistent poor sleep is linked to increased risk of heart disease, insulin resistance, and depression.
In other words, sleep isn’t a passive thing that happens to you. Sleep is an active recovery tool your body depends on. Treating it as a priority is one of the most impactful things you can do for your long-term health in midlife and beyond.
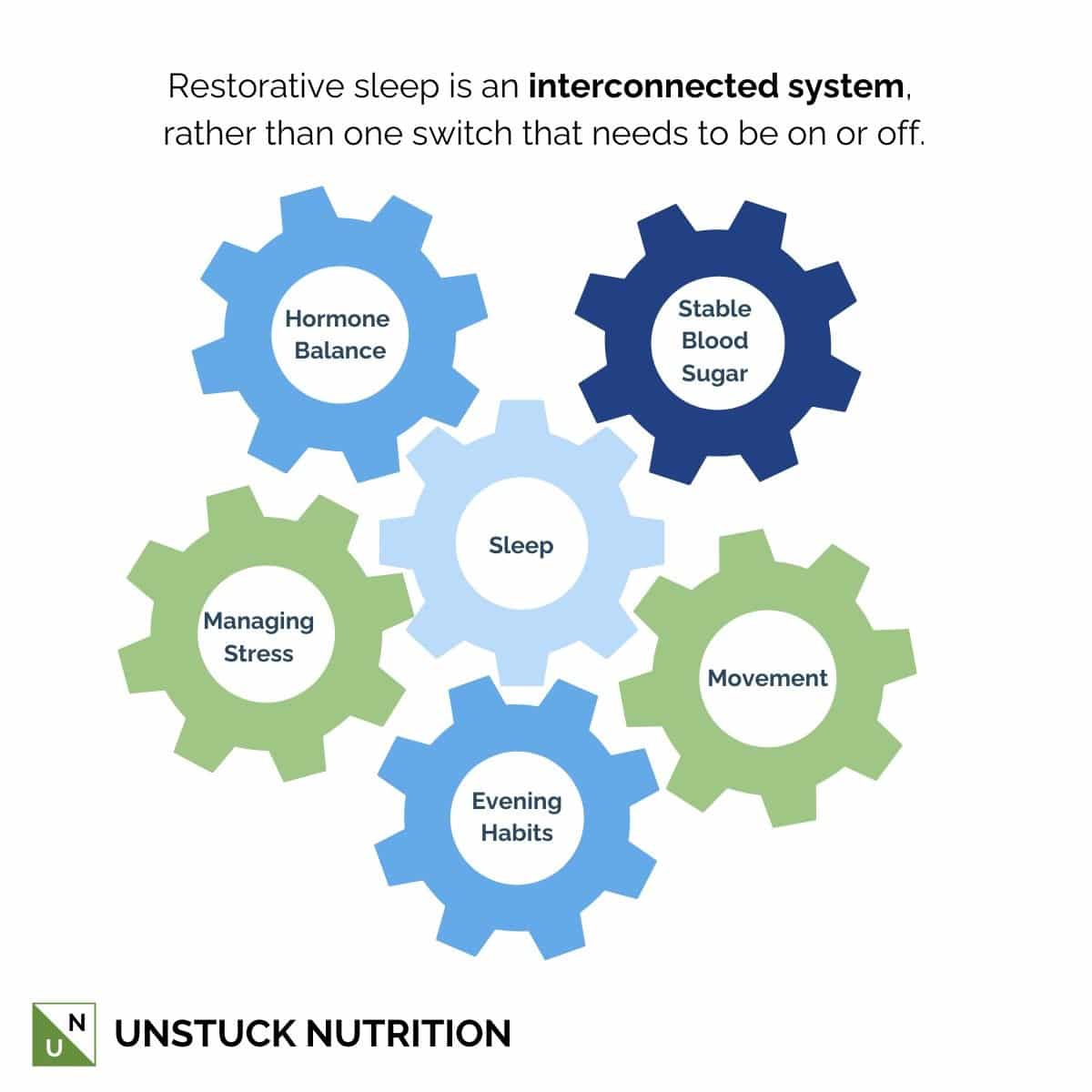
Sleep is a system, not just one switch that needs to be on or off. Better sleep usually comes from adjusting several “knobs” at once: stabilizing blood sugar, managing stress, supporting hormone balance, moving your body regularly, and improving your evening habits.
The Sleep-Inflammation Connection
So, how exactly does poor sleep drive inflammation?
During healthy sleep, your body isn’t simply resting; it’s actively regulating your immune system. Sleep helps you process prior immune challenges, primes your defenses for the next day, and keeps inflammatory activity appropriately timed to nighttime hours. When sleep is disrupted, the coordination breaks down.
What Happens in Your Body When You Don’t Sleep Enough
Research shows that disrupted sleep can cause increased inflammatory signals during the day, leading to low-grade chronic inflammation. At the same time, your immune system’s targeted response weakens, making the body less able to fight off infection and more prone to overreaction. I often notice that after several nights of poor sleep, I am more likely to catch a cold or have migraines. Poor sleep may show up differently for you.
The evidence is especially clear for women in midlife. A study of 281 healthy women aged 45 to 60 found that poor sleep quality and low sleep efficiency were directly associated with elevated levels of key inflammatory markers (CRP and IL-6) and that sleeping less than 5 hours was associated with high CRP levels in menopausal women.
A separate 2024 study of 237 healthy adults found that sleep disruption increased immune cells that prime the body for chronic inflammation, and that these changes reversed when sleep improved.
Even one night of poor sleep can cause a short-term spike in inflammation. The cumulative effect of chronic sleep deprivation, however, significantly increases the risk of inflammatory diseases, including heart disease, insulin resistance, type 2 diabetes, and depression. The encouraging finding across both studies: improving sleep quality reverses these changes, making sleep one of the most direct ways you can reduce inflammation.
The Inflammation-Sleep Cycle
Inflammation and sleep disruption feed each other directly, which is what makes poor sleep challenging to fix.
Poor sleep increases inflammatory markers, and elevated inflammation then fragments sleep further:
- Reducing deep sleep
- Lowering sleep efficiency (time asleep in bed)
- Increasing nighttime wakefulness
Sleep deprivation shifts immune cells toward more inflammatory states, putting them on high alert and making them respond more aggressively to everyday triggers. For women already managing inflammatory or autoimmune conditions, this compounds the effect.
Elevated cortisol is a third driver of this poor sleep-inflammation loop. Chronic sleep disruption elevates cortisol, further disrupting sleep structure and increasing inflammatory signaling. If you haven’t already, it’s worth reading how this cortisol connection plays out in midlife: Stress, Cortisol & Inflammation in Midlife Women
Together, poor sleep, elevated inflammation, and dysregulated cortisol reinforce each other in a hard-to-break cycle, and the shifting hormones during midlife add to it. The good news is that addressing any one of them creates positive momentum and helps interrupt the cycle.
How Poor Sleep Affects Eating and Blood Sugar
There’s a reason you may be drawn to a sugary, caffeinated latte and a baked good after a night of fragmented sleep. When we sleep poorly, our eating habits are negatively impacted! This is why cravings after poor sleep often feel unusually intense. Your hormones and blood sugar regulation are actively shifting in response to sleep deprivation.
Sleep deprivation affects hunger hormones, appetite, food cravings, and even the types of foods you’re most likely to choose.
Research repeatedly shows that inadequate sleep increases ghrelin (a hunger hormone) and decreases leptin (a fullness hormone), driving cravings for more food the next day.
Additionally, researchers found that forced reductions in sleep quality and hours of sleep (-33%, limited to 5 hours) for 8 days increased daily energy intake by 559 calories. The body did not compensate by burning any extra energy, either, making you more prone to weight gain.
A small study found that when 11 adults slept less than 5.5 hours daily for 3 weeks, they ate more snacks and higher-carbohydrate foods. Other larger studies have confirmed that sleep deprivation leads to increased intake of fat- and carbohydrate-rich foods.
A 2022 systematic review found that consistently sleeping less than 7 hours is associated with increased insulin resistance. Over time, this means the body becomes less effective at controlling blood sugar and inflammation, and raises the risk of diabetes.
A bad night of sleep can influence you to consume more inflammatory foods the next day, and chronic poor sleep compounds the effect.
This is one reason why building a balanced, protein-rich breakfast can help stabilize energy, cravings, and blood sugar after a poor night of sleep. → Best Anti-Inflammatory Breakfast Ideas
If you’ve ever wondered how sleep affects your real-time blood sugar patterns, my CGM experiments showed just how dramatically small changes can influence glucose levels. → What Happened to My Blood Sugar When I Cut Evening Snacks
What to Eat After a Poor Night of Sleep
Okay, so you had a terrible night of sleep. Now what?
After a night of fragmented sleep, it’s common to crave sugary foods, oversized coffee drinks, and quick sources of energy. But those choices often lead to blood sugar crashes, worsening cravings, and even more fatigue later in the day.
Focus on stabilizing your blood sugar early.
Start your morning with a breakfast that combines protein, fiber, and healthy fats, such as scrambled eggs with vegetables or unsweetened Greek yogurt topped with berries and nuts. This combination helps keep you full, supports steadier energy levels, and reduces the intense cravings that often follow poor sleep. → Anti-Inflammatory Breakfast Ideas
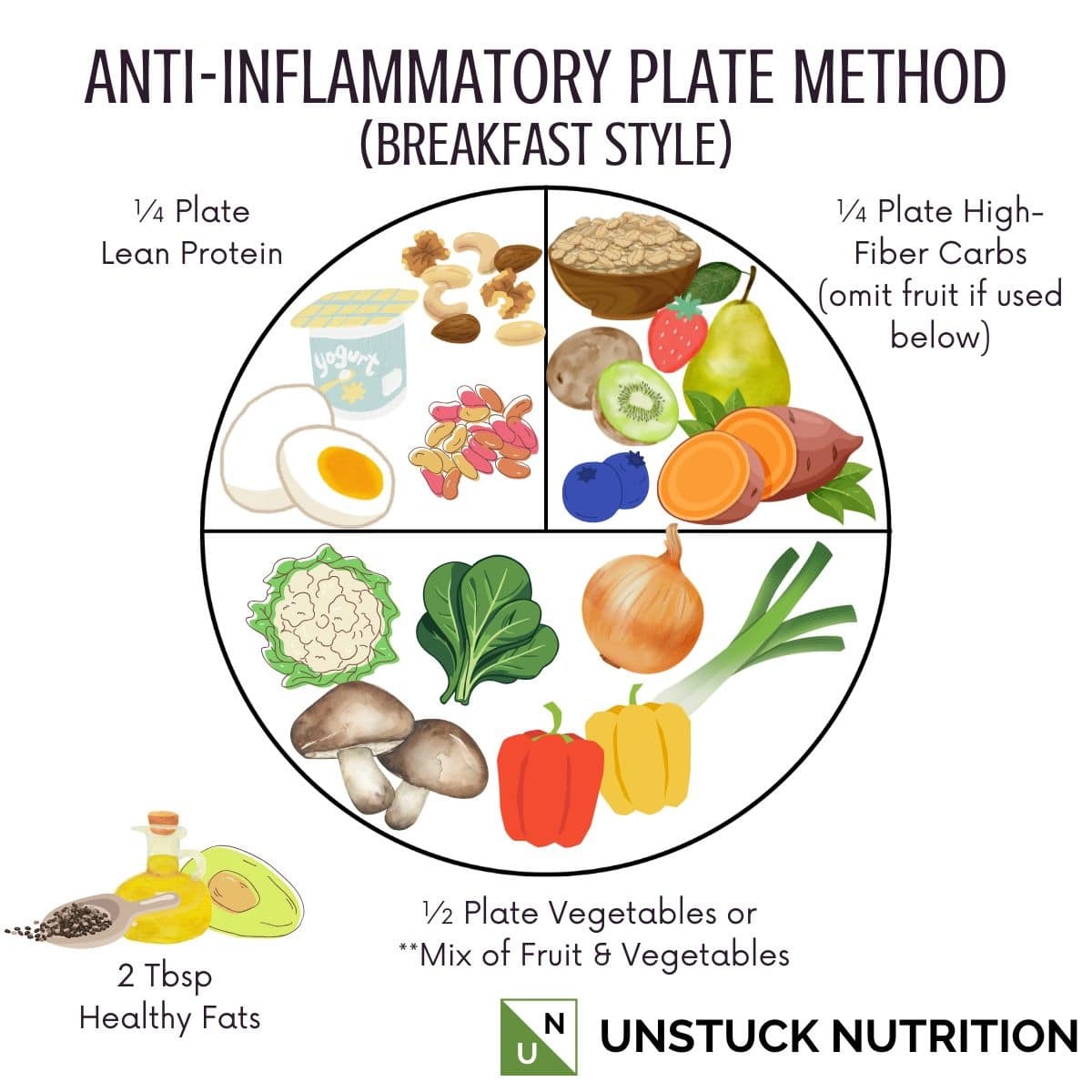
You can also pair breakfast with a lower-sugar caffeinated drink, such as black coffee with half-and-half, cold brew, or a lightly sweetened latte. Having caffeine alongside a balanced meal may help reduce the energy spikes and crashes that can happen when caffeine is consumed on its own.
Coffee can absolutely fit into an anti-inflammatory diet when timing and added sugar are considered. → Mediterranean Diet and Coffee: Can You Drink It?
Hydration matters too. Even mild dehydration can worsen fatigue and increase the likelihood of mistaking thirst for hunger. Water, unsweetened sparkling water, or unsweetened iced tea are all good options to support energy and focus throughout the day.
The goal isn’t perfection after one bad night of sleep. It’s creating enough stability through balanced meals, hydration, and blood sugar support to help interrupt the sleep-stress-inflammation cycle rather than amplify it.
Anti-Inflammatory Foods That Support Better Sleep
Research confirms that what you eat directly influences how well you sleep. A 2016 review in Advances in Nutrition found that higher fiber intake was associated with more time in deep restorative sleep and fewer nighttime wakings, while higher saturated fat and sugar intake were linked to lighter sleep and increased nighttime wakings.
The Mediterranean diet — the same eating pattern most strongly supported for reducing inflammation — was also associated with fewer insomnia symptoms in women specifically, suggesting that anti-inflammatory eating and sleep-supportive eating are largely the same thing.
If you want to learn more about starting an anti-inflammatory diet, like the Mediterranean diet, read my in-depth guide with practical tips on getting started → What is an Anti-Inflammatory Diet? Foods, Benefits, and a Dietitian’s Guide
You can also learn how an anti-inflammatory diet helps in midlife → Anti-Inflammatory Diet for Perimenopause: A Dietitian’s Complete Guide
Nutrients that Support Sleep Quality
Emerging research suggests that certain anti-inflammatory foods may directly support sleep quality and duration.
- Eating 2 kiwifruits 1 hour before bed for 4 weeks significantly reduced the time to fall asleep (by 14 minutes), while improving total sleep time (41 minutes) and sleep efficiency in adults with sleep issues. Plus, two kiwifruits provides 100% of your daily vitamin C needs.
- Fatty fish provides both vitamin D and omega-3 fatty acids, both of which support serotonin regulation and sleep quality.
- Tart cherry juice, when consumed morning and evening, increases melatonin levels, contains natural melatonin, and anti-inflammatory compounds that may help improve sleep quality, total sleep time, and sleep efficiency in multiple studies.
- Higher magnesium levels (and possibly supplementation) are linked to better sleep. Food high in magnesium includes leafy greens, beans, whole grains, chia and pumpkin seeds, and dark chocolate.
- Tryptophan is a precursor to serotonin and melatonin and can support sleep when paired with carbohydrates, but its effects are gradual. Tryptophan supplementation, especially at higher doses, may help reduce nighttime awakenings. Foods include turkey, chicken, eggs, cheese, fish, dairy products, and nuts or seeds (pumpkin especially).
- A 2024 systematic review found that omega-3 fatty acids (from fatty fish, walnuts, and flaxseed) are associated with longer sleep duration and better sleep quality.
Eating Patterns that Affect Sleep
Beyond individual foods, overall eating patterns matter, too.
Following a Mediterranean-style eating pattern rich in fiber, fruits, vegetables, antioxidant-rich foods, omega-3 fats, and adequate protein is associated with better sleep quality and fewer insomnia symptoms.
On the other hand, skipping breakfast and eating irregularly are both associated with poorer sleep quality and greater nighttime waking.
Meal timing matters as well. Large meals high in saturated fat or refined carbohydrates close to bedtime are linked to longer sleep onset and lower sleep efficiency, with women appearing especially sensitive to evening food intake during midlife.
Keeping your last large meal two to three hours before bed and choosing a small, balanced snack, if needed, can help support steadier overnight blood sugar and reduce nighttime wakefulness.
Waking between 2 and 4 am is a common sleep complaint in perimenopausal women, often caused by hormonal shifts and cortisol dysregulation. However, blood sugar drops may also play a role. For some women, a strategic bedtime snack (15 g of fiber-rich carbohydrate + 15 g of healthy fat) can help stabilize overnight blood sugar. Good options include 5-6 strawberries or a small apple with a small handful of nuts or nut butter.
I like to keep these nutrient- and fiber-packed energy bites on hand for a quick bedtime snack. You only need 1 or 2 energy bites paired with some berries.

If you need more ideas, check out my list → 10 Best Anti-Inflammatory Snacks to Buy
Caffeine timing matters as well. Try cutting off caffeine by around 2 pm (roughly 8–10 hours before bedtime), and pay attention to whether caffeine worsens hot flashes or nighttime waking.
Alcohol can also fragment sleep structure, even if it initially makes you feel sleepy. While individual responses vary, many women notice worsened hot flashes, nighttime awakenings, and less restorative sleep after drinking alcohol in the evening.
Lifestyle Habits That Break the Sleep-Inflammation Cycle
The good news is that even small changes in sleep, stress, and blood sugar regulation can begin to improve this cycle surprisingly quickly.
Sleep Hygiene Basics that Actually Matter
Focus on habits that have the greatest impact.
If night sweats or hot flashes are problematic for your sleep, prioritizing a cool bedroom, cotton sheets, and loose pajamas may help you more than they would for someone else. You may need to experiment with caffeine timing and evening alcohol to see if tweaking these improves your symptoms and ultimately, sleep.
Maintain consistent wake times, without much variance on weekends, to create a healthy circadian rhythm that helps your body prepare for sleep each night.
Include morning light exposure within 30 minutes of waking. Natural morning sunlight helps anchor your circadian rhythm and improves your ability to wind down at night.
Movement and Sleep
Research on exercise and sleep in midlife/menopausal women is both consistent and specific! A 2024 meta-analysis found that low- to moderate-intensity aerobic exercise significantly improved sleep in menopausal women. The optimal amount was 3 sessions per week, 70 to 90 minutes each, with improvements seen after 8 to 10 weeks. Start with consistent movement several times per week, if those amounts seem intimidating at first.
The researchers highlighted certain types of exercise. Mind-body forms of exercise, such as yoga, tai chi, and Pilates, outperformed higher-intensity cardio specifically for sleep quality. These exercise styles reduce muscle tension, regulate breathing, lower anxiety, and increase GABA (the brain’s natural calming neurotransmitter).
A separate 2023 systematic review confirmed that yoga and walking showed the greatest improvements in sleep quality and mood among menopausal women.
High-intensity exercise like running or HIIT, while beneficial for other health markers, can actually trigger or worsen hot flashes at higher intensities, which then disrupts sleep. This doesn’t mean avoiding cardio, just plan for morning workouts.
Prioritize yoga, tai chi, pilates, or light walking as your primary movement; add brisk walking on other days; and save higher-intensity workouts for mornings, when they’re less likely to interfere with nighttime sleep.
Movement supports more than sleep alone. Regular exercise lowers inflammation, improves insulin sensitivity, regulates stress hormones, and supports long-term health → Best Ways to Reduce Inflammation: 4 Factors Beyond Food
Stress and Cortisol at Night
The “tired but wired” feeling experienced by many midlife women has a real physiological explanation. As estrogen and progesterone fluctuate and decline during perimenopause, the stress system can become more reactive, allowing cortisol to rise and fall out of normal rhythm.
When cortisol levels remain elevated in the evening (when they should be low), the nervous system stays in a low-grade state of alert, making it harder to fall asleep and stay asleep. Over time, chronically elevated cortisol drives low-grade inflammation and compounds sleep and hormonal symptoms you may already be managing.
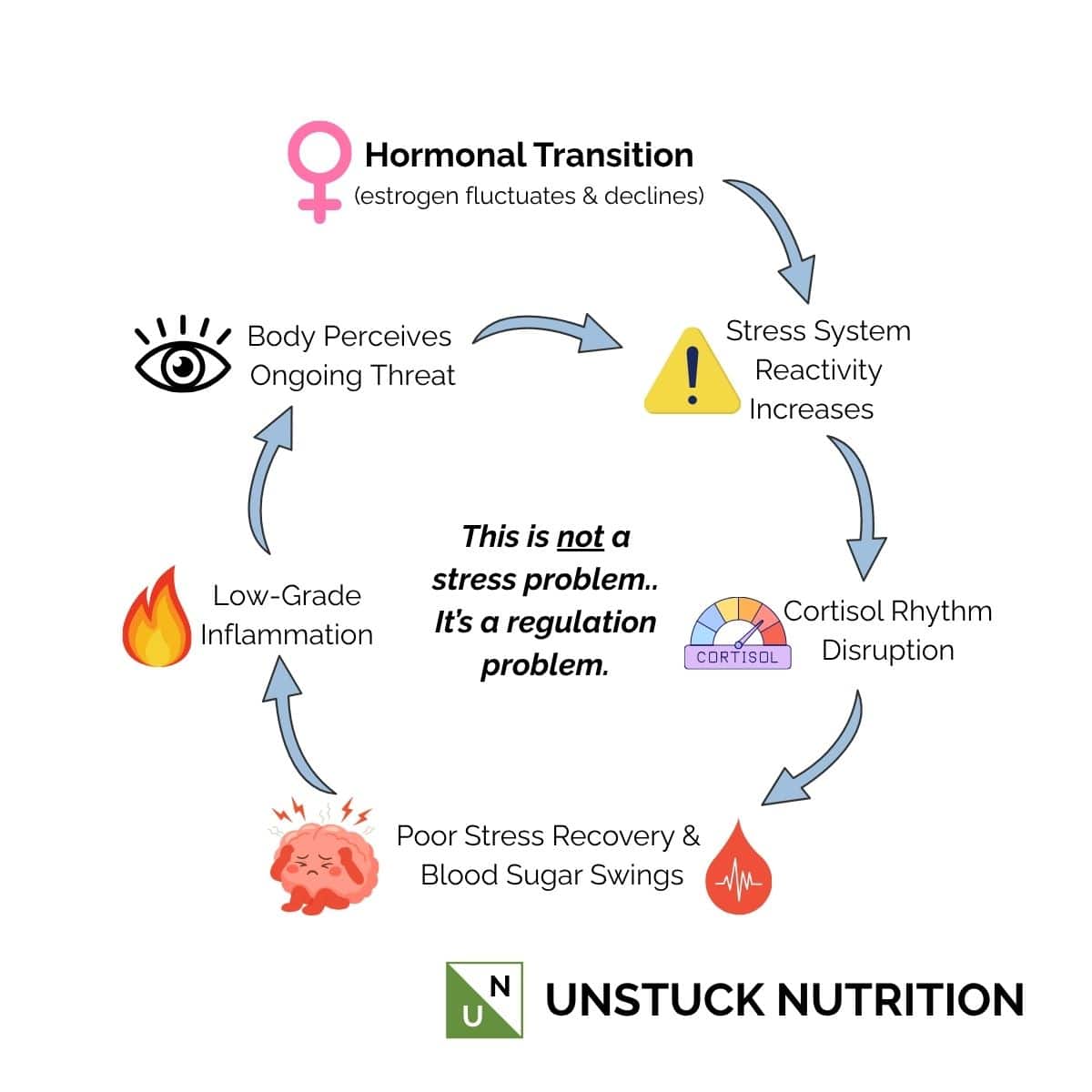
This cortisol-sleep connection is covered in much greater depth, including practical nutrition and lifestyle strategies to restore balance, in → Stress, Cortisol & Inflammation in Midlife Women.
When to Talk to Your Doctor
While poor sleep is common in midlife, several underlying factors are worth ruling out or discussing with your provider, as many are treatable.
Sleep Apnea: Research suggests that 47 and 67% of postmenopausal women have sleep apnea, driven partly by body composition changes (increased belly fat) during the menopause transition. If you snore, wake gasping, feel exhausted despite hours in bed, or notice morning headaches, mention it to your provider. Sleep apnea is treatable and can lead to better sleep and reduced inflammation.
Hormonal Therapy: If you struggle with sleep disruption caused by hot flashes and night sweats, hormone therapy (estrogen and micronized progesterone) is an effective medical treatment. Speak with a healthcare provider knowledgeable about perimenopause to see if this is a good option for you.
Thyroid Function: Thyroid issues, including Hashimoto’s thyroiditis and hypothyroidism, are common and contribute to sleep disruption, fatigue, and mood changes in midlife women. If sleep problems are accompanied by unexplained weight changes, cold intolerance, or brain fog, ask your provider about thyroid screening → Hashimoto’s Thyroiditis Diet: What to Eat + Anti-Inflammatory Guide
Mental Health and Mood: Anxiety and depression increase significantly during the perimenopause transition and impact sleep. If low mood or persistent anxiety seems to be increasing for you, seek help from your provider to help distinguish between hormonal mood shifts and clinical anxiety or depression, which have different treatment paths.
FAQs
Why do I wake up at 3 am every night?
Hot flashes and night sweats often peak in the early morning hours, plus the fluctuating estrogen and progesterone levels during midlife can lead to cortisol dysregulation. When cortisol levels are mis-timed and elevated at night, it can disrupt your normal sleep cycle.
Does poor sleep cause weight gain after 40?
Poor sleep and weight gain are closely related, and the relationship gets stronger in midlife. A study of more than 68,000 women found that those who slept 5 hours or less per night gained significantly more weight over time than those who slept 7 or more hours.
Poor sleep increases hunger hormones and cravings for high-calorie foods, impairs insulin sensitivity, raises cortisol and inflammation, and promotes fat storage in the mid-section. Sleep is an anchor for inflammation and weight management in midlife.
What foods help you sleep better?
Foods that support stable blood sugar and provide nutrients involved in melatonin and serotonin production may help improve sleep quality. Examples include: fatty fish, kiwi, tart cherries, nuts, seeds, leafy greens, yogurt, eggs, and other protein-rich, tryptophan-rich, or magnesium-rich foods.
Eating patterns matter, too. A Mediterranean-style eating pattern rich in fiber, antioxidants, healthy fats, and adequate protein is consistently associated with better sleep and lower inflammation.
How many hours of sleep do women over 40 need?
Most adults, including midlife women, need between 7 and 9 hours of sleep per night for optimal health. During perimenopause and menopause, sleep quality becomes more important. Frequent nighttime awakenings, hot flashes, and lighter sleep can leave you feeling exhausted even if you are meeting the goal of 7 to 9 hours of sleep.
Can the anti-inflammatory diet improve sleep?
Research suggests that anti-inflammatory eating patterns, particularly the Mediterranean diet, are associated with better sleep quality and fewer insomnia symptoms.
Anti-inflammatory foods help keep blood sugar levels stable, reduce inflammation, sustain energy levels, and provide nutrients involved in sleep regulation. Since inflammation and poor sleep reinforce each other, improving diet quality may help support more restorative sleep over time.
Takeaways
Poor sleep in midlife is not “just aging” or a low-priority issue. Hormonal shifts, cortisol dysregulation, inflammation, blood sugar instability, and lifestyle habits all impact how well you sleep and how rested you feel the next day.
The encouraging news is that sleep can improve. The same habits that support an anti-inflammatory lifestyle: balanced meals, stable blood sugar, stress management, movement, and consistent routines, also support restorative sleep.
Learn more about anti-inflammatory foods and their benefits in this guide → What is an Anti-Inflammatory Diet? Foods, Benefits, and a Dietitian’s Guide
Sleep is not a luxury in midlife. It’s a foundation and one of the body’s most important recovery tools. Don’t underestimate the powerful effects of sleep on reducing inflammation, increasing your capacity for movement, and giving you the energy to prepare healthy meals that support long-term wellness. Everything feels a little more manageable after a restful night’s sleep.
If you’ve been feeling stuck in the cycle of exhaustion, cravings, inflammation, and restless nights, remember: you don’t have to fix everything at once. Better sleep is often built through small, consistent changes that work together over time.
Let’s get UNstuck and stay UNstuck — one night of better sleep at a time.