Anti-Inflammatory Diet for Perimenopause
I turn 40 on March 23, 2026.
And over the past few years, I’ve had a front-row seat to how hormones can shift.
In April 2023, I had a partial right nephrectomy due to kidney cancer (resolved now). Two months later, I underwent a full hysterectomy for endometriosis, leaving one ovary intact. While I’m deeply grateful for my health, those surgeries accelerated my awareness of something many women quietly experience in their 40s: inflammation starts to feel different in midlife.
Energy changes.
Moods shift.
Sleep becomes lighter (or at least more sensitive).
Weight redistributes.
Blood sugar is less predictable.
Joint stiffness appears or increases.
As a registered dietitian, I knew the science behind inflammation. But living through hormonal shifts made the research personal.
Perimenopause is not just about hot flashes and missed periods. It’s a time of fluctuating estrogen, increased metabolic vulnerability, and often rising low-grade inflammation.
The good news? Nutrition can make a meaningful difference. An anti-inflammatory diet is a way of eating that focuses on whole, minimally processed foods to help reduce chronic, low-grade inflammation in the body.
In this guide, I’ll walk you through:
- Why inflammation may increase during perimenopause
- How hormone fluctuations affect metabolism
- The best anti-inflammatory foods for women in midlife
- What to reduce (without extreme dieting)
- And how to structure meals to support hormone balance and steady energy
This isn’t about restriction.
It’s about building a sustainable anti-inflammatory foundation that supports your body through midlife and beyond.
Let’s break it down.
→ If you want to jump directly to a clear, organized anti-inflammatory diet guide, download my printable anti-inflammatory food list (what to eat more of and what to limit)
What Happens to Hormones During Perimenopause?
Let’s first define what menopause and perimenopause are, since hormones are a driving force for each stage.
Menopause is the permanent stopping of menstruation, confirmed after 12 consecutive months of no menstrual cycles. Ideally, menopause occurs between the ages of 45 and 55.
Menopause may sound appealing, not having to deal with monthly cycles, but there are adverse effects of an early transition. Early menopause (before age 45) significantly increases risks of heart disease, stroke, osteoporosis, cognitive health, cancer risk, and mood instability due to prolonged estrogen deficiency.
The transition period leading up to this is perimenopause, which typically begins in the mid-to-late 40s and may last four to eight years. The longer time frame and uncertainty make this phase harder to predict, making it harder to know when you will officially enter menopause.
Hormones & Perimenopause and Menopause
During this time between normal menstrual cycles, perimenopause, and menopause, your body experiences fluctuating ovarian function and gradual hormonal shifts marked by:
- Declining estrogen levels
- Reduced progesterone levels
- Increased FSH and LH (gonadotropins) due to increased production from the brain that signal the ovaries to produce estrogen, progesterone, and release eggs.
As you enter perimenopause, you will start to notice these hormonal shifts and their effects on your entire body, ranging from hot flashes, night sweats, sleep disruption, mood swings, vaginal dryness, worsened metabolic and bone health, and increased systemic inflammation (plus many more).
Additionally, before menopause, women are generally more protected against metabolic conditions such as insulin resistance, diabetes, and heart disease, but this effect disappears at menopause due to changing hormone levels.
This shift means that your body becomes more vulnerable to changes in metabolism, blood sugar, and inflammation, often before you even notice obvious symptoms.
You can think of it like this:
hormonal changes → increased inflammation → reduced insulin sensitivity → increased fat storage and symptoms.
A 21-year longitudinal study of 1,470 midlife women (aged 42-52) found that systemic inflammation (CRP and IL-6) often rises around the menopause transition, beginning about one year before the final menstrual period, particularly in women with higher body weight, but all women experienced this, suggesting menopause contributes to long-term inflammatory disease risk.
For a deeper look at how blood sugar connects to cortisol and inflammation, read my in-depth article on stress, cortisol, and inflammation in midlife women, where I break down key signs of imbalance and share practical nutrition and lifestyle strategies to help restore balance.
You may be wondering what predicts the start of this transition to better support your health.
Factors That Influence the Timing of Menopause
Researchers examined factors that predict the onset of natural menopause in 279 pre- and perimenopausal women aged 47-55 years. The average age at menopause was 52.8 years old. The 2021 study evaluated 32 potential predictors and identified the most useful and impactful.
Several predictors of approaching menopause include:
- Reproductive Hormone Levels: the strongest predictor, often higher follicle-stimulation hormone (FSH) and higher estrogen levels right before transition.
- Family History or Genetics: women whose mothers experienced early menopause are at a higher risk of early menopause themself.
- Menstrual Cycle Changes: greater variability in cycle length and/or irregular menstrual bleeding are associated.
- Diet and Eating Patterns: pro-inflammatory diets (high intake of processed foods and carbs) are linked to an increased risk of early menopause, whereas an anti-inflammatory diet (fish, lean protein, beans, vegetables, fruit, and vegetarian) is associated with a later menopause.
- Menopausal Symptoms: hot flashes and night sweats, but usually later symptoms
- Lifestyle Factors: higher alcohol intake as women neared menopause, smoking causes earlier menopause by accelerating ovarian aging and damage. At the same time, regular physical activity is associated with healthier hormone regulation and slightly later menopause.
- Social Factors: higher education level often correlates with better healthcare access and may slightly affect timing (not a strong predictor), whereas relationship status was assessed and was not a strong predictor either.
- Reproductive Variables: the use of hormonal contraceptives could influence ovarian aging, but was not a strong predictor in this study. Some other research indicates that tubal ligation carries a slightly higher risk of earlier menopause. Fertility treatments (injectable FSH and LH, Clomid, and Letrozole) that cause ovarian overstimulation may be a risk factor for earlier menopause (women entered menopause at 43.8 years in this study).
While you can’t control every factor that influences menopause timing, many of these, especially diet and lifestyle, are areas where small, consistent changes can make a meaningful difference.
While researchers study predictors of menopause, each person’s experience is unique.
Making lifestyle changes before perimenopause and menopause can help set the stage for a smoother transition. Whether it’s managing daily changes and reducing annoying and unpleasant side effects like hot flashes and mood shifts, or thinking big-picture, such as taking steps to reduce inflammation and improve long-term health.
Nutrition and lifestyle changes can make a meaningful difference in helping you feel your best as you age through midlife and beyond. And remember it’s more about overall diet quality, not just single foods, that helps your body reduce inflammation and optimize whole-person health.
Does Inflammation Increase During Perimenopause?
Low-grade inflammation tends to increase during the menopause transition and into early postmenopause. In a 21-year study of 1,470 women, markers of inflammation (CRP and IL-6) began rising about a year before the final menstrual period and continued afterward. Although increases were greater in women with higher body weight, all women experienced some rise, suggesting menopause may contribute to long-term disease risk through increased inflammation.
This means that even if you feel relatively healthy, underlying inflammation may already be increasing, making this a critical time to take a proactive approach.
Different Inflammation Patterns
Not every woman experiences menopause the same way. The study identified different inflammation trajectories:
- Low-level inflammation that increases during menopause
- Stable inflammation over time
- High inflammation that stays high or declines
Women starting with low to moderate inflammation were more likely to see a rise during the transition, while those with overweight or obesity often began with high inflammation that persisted.
In other words, there isn’t one ‘normal’ menopause experience; your baseline health and lifestyle play a major role in how inflammation shows up for you.
Why Inflammation Matters
The cytokine IL-6 and acute-phase C-reactive protein (CRP) are widely used inflammatory markers. Higher levels of CRP and IL-6 are associated with aging and predict poorer physical and cognitive performance, as well as increased mortality risk. Chronic, low-grade inflammation is a key factor in long-term health risks, making this period especially important for preventive strategies.
Role of Estrogen
Estrogen helps regulate inflammation by maintaining immune balance. As estrogen declines during perimenopause and menopause, this anti-inflammatory protection decreases, contributing to a rise in chronic inflammation.
Body Composition Changes
Menopause often brings changes in body fat distribution, particularly increased abdominal fat. This fat produces inflammatory signaling molecules called adipokines, which further promote inflammation and may increase long-term disease risk. A 2024 meta-analysis confirmed these changes when comparing pre- and postmenopausal women.
Lifestyle Factors: Sleep and Stress
Poor sleep and chronic unmanaged stress can amplify inflammation during menopause.
- Poor sleep is associated with increased levels of inflammatory markers such as CRP and IL-6.
- Chronic stress can lead to cortisol resistance and a heightened inflammatory response.
As estrogen declines, women may become more vulnerable to these inflammation-promoting pathways.
This is why focusing only on food isn’t enough. Sleep and stress management are key pieces of reducing inflammation during midlife.
The menopausal transition is a critical window during which inflammation increases in almost all women, making it a powerful time to prioritize an:
- Anti-inflammatory diet
- Healthy sleep patterns
- Effective stress management
- Weight management
…to reduce inflammation and support long-term health and well-being.
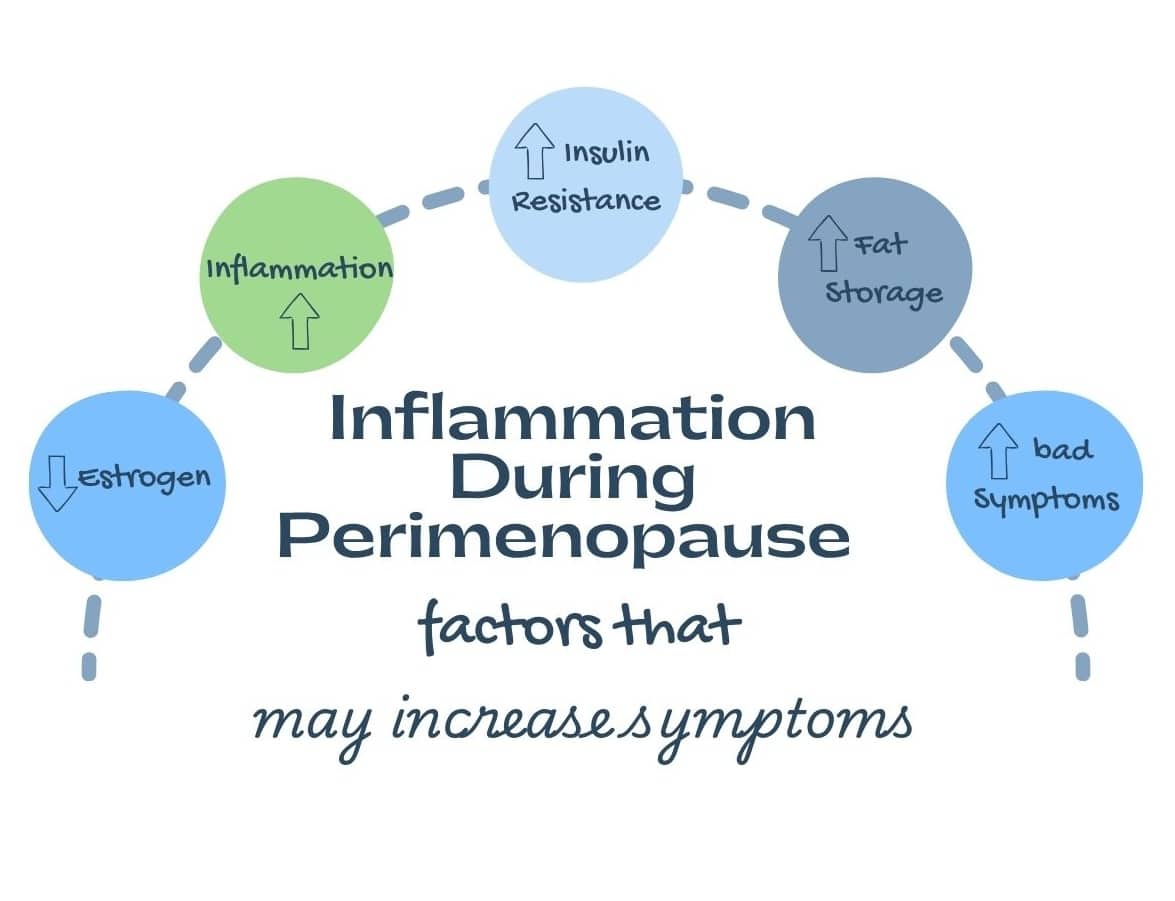
Together, these changes create a perfect storm for rising inflammation during midlife, often without obvious warning signs. Combined, the changes in estrogen, rising inflammation, and redistribution of body fat set the stage for the weight changes women often notice after 40, making this next topic especially relevant.
Why Weight Gain Feels Different After 40
As you near midlife, you may notice that weight gain is different from what you experienced throughout the rest of your adulthood. Maybe you could make some specific changes and return to a stable, appropriate weight for your body size. Now, weight gain is easy and may not be caused by any specific change in your eating habits or physical activity.
A combination of general aging, hormonal changes, lifestyle changes, and more drives weight gain in midlife. Plus, weight gain may be more noticeable in the midsection (fat redistribution), or perhaps you notice a reduction in muscle mass.
Here’s why weight gain feels different in midlife:
1. Aging and Slower Metabolism
Everyone loses muscle mass as they age, including women. Less muscle mass equates to a lower resting metabolic rate. At the same time, you require less energy as you age, since your body is no longer growing, and you are more in recovery/maintenance mode.
So you are burning less energy and requiring less energy intake, making it easier to gain weight without any major changes in eating habits. Research shows that on average, women gain about 1.5 pounds per year during midlife.
At the same time, many women notice a gradual decline in physical activity, further reducing their daily calorie burn.
2. Hormonal Changes (Estrogen Decline)
Menopause itself doesn’t cause significant weight gain, but declining estrogen levels shift your body composition toward more body fat and promote abdominal (visceral) fat storage, which is more metabolically active and can increase inflammation right by your internal organs.
This means more fat mass, decreased lean (muscle) mass, and more central body fat distribution. The scale may not change drastically, but weight may feel different at midlife. Your waistband may gradually feel tighter, or you find you need looser clothes in your mid-section to be comfortable.
3. Sleep Disruption
Sleep disturbances (often from night sweats, mood changes, or hormonal shifts) are linked to increased weight gain, partly due to fatigue, which reduces activity levels. This may not occur until closer to menopause.
In a study of more than 68,000 women, those who slept 5 hours or less gained more weight than those who slept more than 7 hours each night.
4. Mood and Stress
Mood changes, which affect up to one-fourth of perimenopausal and postmenopausal women, can also interfere with the ability to adopt healthy lifestyle habits and contribute to weight gain through emotional eating or reduced motivation for physical activity.
5. Blood Sugar Variability
Changes in blood sugar regulation can make weight gain feel more pronounced during midlife.
Estrogen helps deliver glucose to the muscles and suppresses glucose production in the liver. It also helps regulate lipid levels in the body and prevents the accumulation of body fat, particularly around the abdomen.
As estrogen declines, the body can become less sensitive to insulin, increasing the likelihood of blood sugar spikes and crashes. These fluctuations can lead to increased hunger and cravings for quick carbs, energy dips, which reduce motivation for movement, and promote fat storage.
Long-term blood sugar variability can lead to higher insulin levels and increased inflammation. Inflammation worsens insulin resistance, and so the cycle continues. This cycle of blood sugar swings and inflammation can make it feel like your body is working against you, but it’s also one of the most responsive areas to nutrition changes.
You were right in feeling that weight gain feels different in midlife! This is why traditional approaches to weight loss often feel less effective during midlife: the underlying drivers have changed.
Your body is changing drastically, and this is exactly where an anti-inflammatory diet can make a meaningful difference and support you during this next stage.
The Anti-Inflammatory Diet Explained
An anti-inflammatory diet is not a specific meal plan, but a pattern of eating that reduces chronic, low-grade inflammation in the body.
Midlife is a prime time frame where inflammation can easily get out of control and lead to bigger health consequences and unpleasant side effects of peri- and menopause.
An anti-inflammatory diet can help downregulate the natural inflammatory response during midlife. An anti-inflammatory diet focuses on eating:
- Large amounts of vegetables and fruit (high in filling and blood-sugar stabilizing fiber)
- Whole foods (fruits, vegetables, beans, whole grains, nuts, and seeds)
- Foods with healthy fats, like olive oil (omega-3 fats and unsaturated fats)
- Low to moderate intake of animal products (dairy, poultry, and eggs) with a focus on fish to stabilize blood sugar, keep you full, and support muscle development
- Foods rich in antioxidants, which help neutralize free radicals and reduce inflammation
- Limited red meat and processed meat
- Minimal added sugars and sodium
There is not ONE anti-inflammatory diet. You can modify this diet to fit your needs and ability to make changes. Starting with eating more whole or real foods (minimally processed) is a simple way to include more anti-inflammatory foods.
Diets that typically follow an anti-inflammatory approach include:
- Mediterranean Diet
- DASH (Dietary Approaches to Stop Hypertension) Diet
- Vegetarian or Flexitarian Diet
- MIND Diet
Research consistently shows that an anti-inflammatory eating pattern is associated with lower levels of key inflammatory markers (CRP and IL-6), regardless of weight loss. Studies in menopausal women also reveal improvements in weight, cholesterol, and blood pressure, indicating improved metabolic health.
Evidence on specific menopausal-symptom relief is still emerging. Still, higher adherence to a Mediterranean diet is linked to fewer symptoms and severity (hot flashes, mood, and disrupted sleep) and better overall health.
On the other hand, pro-inflammatory diets are linked to higher levels of inflammatory markers and poor cognitive function in menopausal women, suggesting dietary inflammation may impact brain health alongside metabolic health.
A more inflammatory diet has also been linked to a 20–30% higher risk of fractures in midlife women compared to those eating an anti-inflammatory diet, even when bone density is normal, highlighting the role of inflammation in bone health.
Research on the “big picture for all adults” shows that anti-inflammatory dietary patterns are associated with:
- ↓ 20% lower levels for key inflammatory markers (CRP and IL-6)
- ↓ 25-30% lower risk of heart disease
- ↓ 30% lower risk of heart attack or stroke
- ↓ 20% reduced risk of type 2 diabetes
- ↓ 20% reduction in overall mortality
- ↓ 20 to 35% lower risk of cognitive decline or Alzheimer’s disease
Now that you understand why an anti-inflammatory approach matters, let’s get practical, starting with the specific foods that can help support your body during perimenopause and menopause.
The good news is that even small shifts toward an anti-inflammatory eating pattern can start to improve these underlying processes.
Best Anti-Inflammatory Foods for Perimenopause
Putting this into practice starts with the foods you choose to eat every day and how to fill your plate in a balanced way. Instead of focusing on restriction, start by adding in key foods that help lower inflammation, support metabolism, fuel your body, and keep blood sugar steady during menopause.
1. Fiber-Rich Foods (Legumes, Vegetables, Whole Grains)
Why? A high-fiber diet (about 21-25+ grams daily) helps support stable blood sugar and reduce inflammation, both of which lower the severity of menopausal symptoms. Fiber-rich foods are packed with anti-inflammatory polyphenols.
2. Healthy Fats (Extra Virgin Olive Oil, Nuts, Seeds)
Why? Extra virgin olive oil (EVOO) is about 70-80% monounsaturated fat (which lowers LDL cholesterol and supports heart health), and it contains polyphenols (like oleocanthal) that have anti-inflammatory effects similar to ibuprofen.
In menopausal women, regular EVOO consumption was associated with fewer psychological symptoms (mood, anxiety, and irritability). Other research suggests that 1-3 tablespoons per day is a good starting point.
Research shows that nuts, especially when combined with the Mediterranean Diet, improve menopausal symptoms over 2 years. While specific amounts were not linked to symptom reduction in this study, research-based Mediterranean diet patterns typically include about one small handful (≈1 ounce or 30 grams) of nuts daily.
3. Phytoestrogen Foods (Soy, Flax, Legumes)
Why? Certain foods contain naturally occurring plant compounds (phytoestrogens) that mimic the effects of estrogen by binding to estrogen receptors. Effects vary by individual, but they can help reduce the frequency of hot flashes and night sweats.
Plus, diets high in legumes are associated with lower overall symptom severity in menopause.
4. Polyphenol-Rich Foods (Vegetables, Fruits, Olive Oil)
Why? Higher adherence to a Mediterranean-style diet is associated with significantly lower menopausal symptom severity, and intervention studies suggest symptom scores may decrease by around 25% with consistent dietary changes.
Rather than focusing on single foods, research consistently shows that regularly including specific types of foods, like olive oil, nuts, legumes, and vegetables, in meaningful amounts is what drives the benefits of an anti-inflammatory diet. The serving sizes below are based on Mediterranean diet research, including large clinical trials like PREDIMED.
Let’s jump into some of the best anti-inflammatory foods. You might be surprised that you are already using many of these!
Best Anti-Inflammatory Foods (+ Serving Size) for Perimenopause
| Food Group | Serving Size | Key Benefits | How It Helps During Perimenopause and Beyond |
| Extra Virgin Olive Oil (EVOO) | 1–3 tablespoons/day | Reduces inflammation, supports heart health | Rich in polyphenols that help lower CRP and IL-6 and may support mood |
| Nuts (walnuts, almonds, hazelnuts) | ~1 oz (small handful) daily | Improves metabolic health, reduces inflammation | Healthy fats help stabilize blood sugar and reduce abdominal fat gain |
| Vegetables (especially leafy greens) | 3–5+ servings/day | High in fiber, antioxidants | Supports gut health, estrogen metabolism, and reduces inflammation |
| Fruits (especially berries) | 1–3 servings/day | Rich in polyphenols | Helps reduce oxidative stress and supports brain health |
| Legumes (beans, lentils, chickpeas) | 3–4+ servings/week | Improves blood sugar, reduces inflammation | Linked to lower menopausal symptom severity and better metabolic health |
| Fatty Fish (salmon, sardines, tuna, mackerel) | 2–3 servings/week | Omega-3 fats reduce inflammation | Supports heart health, brain function, and may reduce joint pain |
| Lean Protein (eggs, poultry, yogurt, tofu) | 20–30g per meal | Supports muscle maintenance and energy levels | Helps offset age-related muscle loss and keeps you full longer |
| Whole Grains (oats, quinoa, brown rice) | 1–3 servings/day | Fiber + steady energy | Helps regulate blood sugar and reduce insulin resistance |
| Soy Foods (tofu, edamame, tempeh) | 1–2 servings/day | Contains phytoestrogens | May help support hormone balance and reduce hot flashes |
| Flaxseed (ground) | 1–2 tablespoons/day | Fiber + lignans | Supports estrogen metabolism and digestive health |
| Herbs & Spices (turmeric, cinnamon, ginger) | Use daily | Anti-inflammatory compounds | Help reduce inflammation and support metabolic health |
| Green Tea (unsweetened) | 1–3 cups/day | Antioxidants (catechins) | Supports metabolism, brain health, and inflammation balance |
You don’t need to overthink every meal to eat this way.
If portion sizes feel overwhelming or you just want a simple way to pull meals together, this is the method I personally rely on. My balanced anti-inflammatory plate takes the guesswork out and helps you build nourishing meals quickly.
This approach combines principles of blood sugar balance, anti-inflammatory nutrition, and practical meal building for everyday life.
Now that you know which foods to focus on, the next step is putting them together in a way that actually works in real life.
How to Build an Anti-Inflammatory Plate for Perimenopause
You don’t need to follow a strict meal plan (that sucks the joy out of life) to eat in a way that supports your body during perimenopause.
→ I walk through how to apply this step-by-step flexible framework to use at any meal: planning meal with the plate method
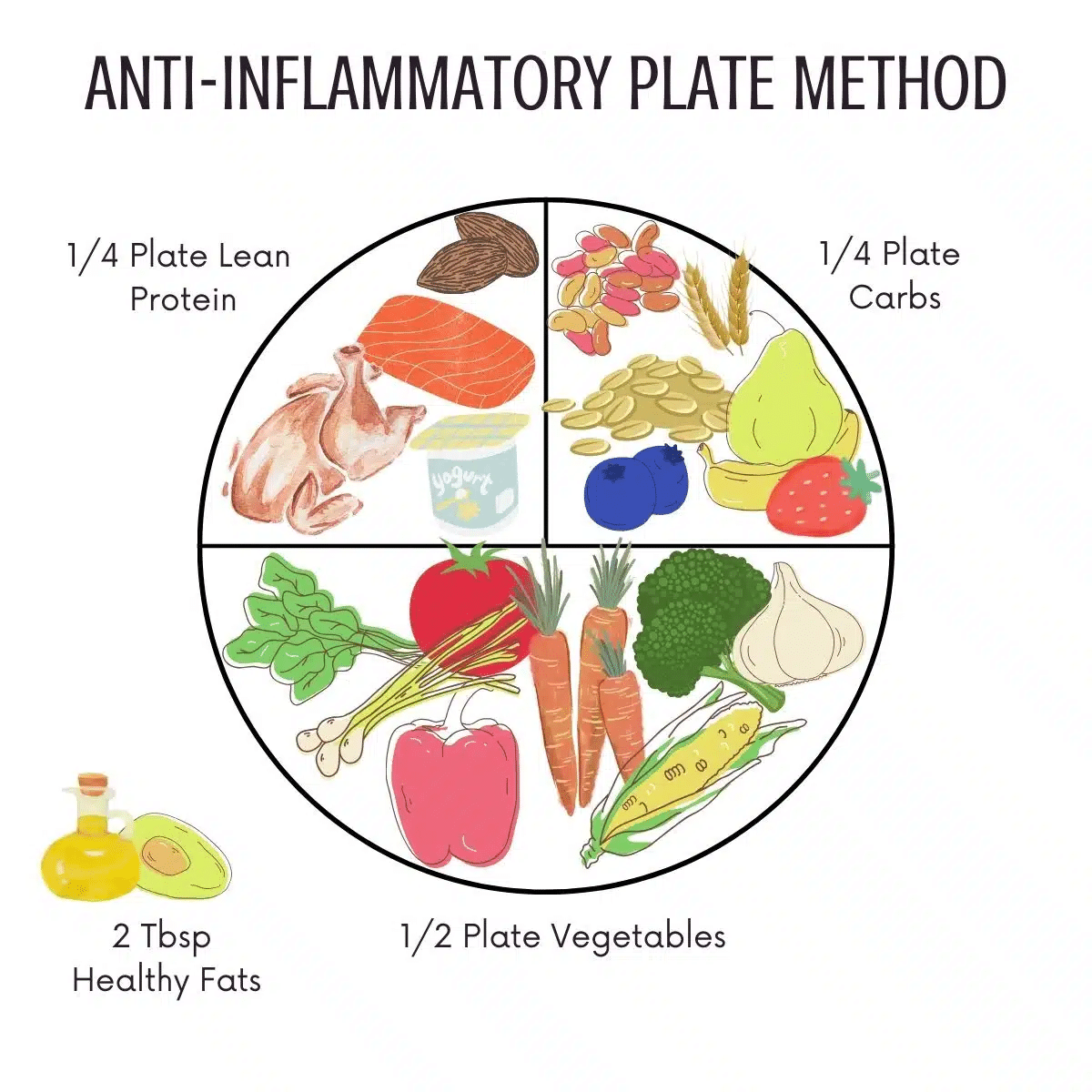
Step 1: Start with Vegetables (½ your plate)
Fill half your plate with a variety of vegetables, especially leafy greens, cruciferous vegetables, and colorful options (deep yellow and orange).
Why it matters: Vegetables provide fiber and antioxidants that help lower inflammation and support gut and hormone health.
Step 2: Add Lean Protein (¼ of your plate)
Include a source of protein, such as fish, chicken, eggs, Greek yogurt, tofu, or beans.
Why it matters: Protein supports muscle maintenance, keeps you full, and helps stabilize blood sugar.
Step 3: Include Smart Carbohydrates (¼ of your plate)
Add whole grains, fruit, or starchy vegetables like sweet potatoes or beans.
Why it matters: Fiber-rich carbohydrates provide steady energy and help prevent blood sugar spikes and crashes, preventing cravings and unnecessary snacks.
Step 4: Don’t Forget Healthy Fats
Add 1–2 tablespoons of healthy fats, such as olive oil, avocado, nuts, or seeds.
Why it matters: Healthy fats help reduce inflammation and support hormone production and brain health.
What This Plate Does for Your Body
When you build meals this way, you naturally support:
- More stable blood sugar (fewer energy crashes and cravings)
- Reduced inflammation
- Better hormone balance
- Improved fullness and satisfaction after meals
Real-Life Sample 1-Day Anti-Inflammatory Meal Plan
- 3 to 4 ounces of grilled salmon (30 grams of protein)
- 1 cup of roasted broccoli + carrots (vegetables)
- ½ cup of quinoa or lentils (carbohydrates)
- 1 tablespoon of olive oil drizzled on the veggies + sliced avocado to top quinoa (healthy fats)
Keep It Flexible
Not every meal has to be perfect. The goal is consistency over time, not perfection. Even loosely following this structure can make a meaningful difference in how you feel. And remember, if you make a mixed dish like a soup or a protein-and-rice bowl, follow the plate method proportions for a balanced meal. Here are some more anti-inflammatory meal ideas!
Now that we’ve discussed foods to make up most of your diet, here are some foods that are linked to increased inflammation.
Foods That May Worsen Inflammation During Perimenopause
Ultra-processed foods and Western dietary patterns are linked with higher inflammatory markers and a greater risk of chronic inflammation. Most nutrition research focuses on the general population rather than menopause.
However, during menopause, you may experience greater blood sugar variability and insulin resistance, which can contribute to inflammation. Research shows that low-grade inflammation tends to increase during the menopause transition and into early postmenopause.
A large NHANES analysis of over 9,000 U.S. adults found that those consuming the highest amounts of ultra-processed foods (60–79% of total intake) had significantly higher CRP levels compared to those consuming the least (0–19%). Even moderate intake levels (40-59%) were associated with higher inflammation.
This means ultra-processed foods can strongly impact inflammation. It also means lowering your intake can help reduce systemic inflammation and your risk for metabolic and heart health issues.
The most favorable group was still consuming up to 19% of their diet with ultra-processed foods. This powerful reminder can help you keep anti-inflammatory vs. inflammatory foods in perspective; overall eating patterns matter more than single food choices.
Rather than focusing on individual foods, it’s helpful to look at eating patterns consistently linked to higher inflammation.
With that in mind, aim to consume less of these inflammatory foods:
Processed and High-Fat Meats
- Bacon
- Hotdogs
- Salami, bologna
- Organ meats
- High-fat red meats
Why it matters: Often higher in omega-6 fats, which, in excess relative to omega-3 fats, stimulate inflammation; if high in saturated fats, this increases inflammation in the gut and colon. Processed meats contain nitrites, which have inflammatory effects.
Added sugars
- Soda, punch, lemonade
- Sports drinks
- Sweetened coffee and teas
- Candy, jams, jellies, syrup, or honey
Why it matters: These can trigger blood sugar spikes, leading to repeated inflammation across all body systems.
Refined grains
- White bread, bagels, rolls
- Crackers and tortillas
- Sugary breakfast cereals (cold and cooked)
- Baked goods (cookies, cakes, donuts, pastries)
Why it matters: They are low in fiber and can quickly raise blood sugar, contributing to inflammation over time.
→ If deciding what to eat for breakfast is overwhelming, this guide walks you through how to build a simple anti-inflammatory breakfast that supports energy and hormone balance
Fried Foods
- French fries, onion rings,
- Fried chicken, meat, or fish
- Chicken nuggets
Why it matters: Often high in unhealthy fats (omega-6 and saturated fats) that promote inflammation when consumed frequently.
Alcohol (Excess Intake)
- Sugary mixed drinks
- Frequent or high alcohol intake
Why it matters: Alcohol can inflame the gastrointestinal tract and promote inflammation in the whole body.
Ultra-processed foods (packaged and ready-to-eat foods)
- Frozen pizza, instant noodles, soups, and packaged meals
- Chips, crackers, cheese puffs
- Mass-produced baked goods and desserts, ice creams
- Condiments and sauces
- Flavored yogurts with added sugars
- Sugary drinks
- Processed meats
Why it matters: These foods often combine added sugars, refined grains, and processed fats—making them a major contributor to dietary inflammation.
The goal isn’t to eliminate these foods completely, but to reduce how often they show up in your daily eating pattern. Small shifts over time can make a meaningful difference in inflammation, energy, and overall health during perimenopause.
At this point, you might be wondering how to apply this in real life. Here are some of the most common questions I hear from women navigating perimenopause and inflammation.
Frequently Asked Questions About Anti-Inflammatory Diets and Perimenopause
1. Can an anti-inflammatory diet help with perimenopause symptoms?
Yes, research suggests that anti-inflammatory dietary patterns are associated with fewer and less severe menopausal symptoms, including hot flashes, mood changes, and disrupted sleep. While results vary, improving overall diet quality can support hormone balance, reduce inflammation, and improve how you feel day to day.
2. Why does inflammation increase during perimenopause?
Inflammation tends to increase during perimenopause due to declining estrogen levels, which normally help regulate the body’s inflammatory response. At the same time, changes in body composition, blood sugar regulation, sleep, and stress can further contribute to chronic low-grade inflammation.
3. Why does weight gain feel different after 40?
Weight gain in midlife is influenced by a combination of factors, including hormonal changes, muscle loss, slowed metabolism, and increased insulin resistance. Fat is also more likely to be stored in the abdominal area as estrogen declines, an area that is more metabolically active and linked to higher inflammation.
4. How does blood sugar affect inflammation during perimenopause?
Blood sugar variability can increase inflammation by triggering repeated spikes and crashes in insulin levels. As estrogen declines, the body may become less sensitive to insulin, making stable blood sugar even more important for reducing inflammation, energy crashes, and cravings.
5. What are the best anti-inflammatory foods for women over 40?
Some of the most effective anti-inflammatory foods include:
- Vegetables and fruits (especially leafy greens and berries)
- Extra virgin olive oil
- Nuts and seeds
- Fatty fish (like salmon and sardines)
- Legumes and whole grains
- Soy foods and flaxseed
These foods provide fiber, healthy fats, protein, and antioxidants that help regulate inflammation and support overall health.
By now, you have a strong foundation for reducing inflammation and supporting your body during perimenopause.
But knowing what to do and consistently putting it into practice are two different things, especially during a busy season of life.
Should You Try a 30-Day Reset?
A 30-day reset isn’t about restriction or starting over; it’s about creating a short, focused period to build consistent habits.
By temporarily simplifying your food choices and prioritizing anti-inflammatory foods, you can begin to stabilize blood sugar, reduce inflammation, and better understand how your body responds to what you eat.
I’m currently creating a guided 30-day reset to make this process simple and sustainable. If you’d like to be the first to know when it’s available, you can join my newsletter here.
In the meantime, you can start by:
- Using the anti-inflammatory plate method
- Adding 1–2 anti-inflammatory foods to each meal
- Gradually reducing ultra-processed foods with some simple swaps
Takeaways
Perimenopause is a time of significant change, but it’s also a powerful opportunity to support your body more intentionally.
As estrogen levels shift, inflammation, blood sugar regulation, and body composition can change. These changes can affect energy, weight, mood, and overall health, but they are not out of your control.
The most important takeaway is this: you don’t need a perfect diet—you need a consistent pattern.
Focusing on whole, anti-inflammatory foods, building balanced meals, and reducing ultra-processed foods over time can help:
- Support more stable energy and fewer crashes
- Improve blood sugar balance and reduce cravings
- Lower chronic, low-grade inflammation
- Support long-term metabolic, heart, and brain health
Start simple:
- Build meals using the anti-inflammatory plate method
- Add more vegetables, healthy fats, and fiber-rich foods
- Reduce ultra-processed foods gradually—not all at once
Small, consistent changes add up—and this is where real progress happens.
You don’t need to overhaul everything overnight. Start with a few small shifts, build balanced meals, and stay consistent over time.
Let’s get UNstuck and stay UNstuck—supporting your body through perimenopause, one meal at a time.